Struggling to figure out how to get rid of bacne can be frustrating, especially when the back is one of the hardest places to treat. In this guide we break down the science behind back acne, outline practical daily routines, and explore both over‑the‑counter and professional treatments that deliver lasting results. Whether you’re dealing with occasional breakouts or persistent inflammation, understanding the root causes will empower you to take control of your skin health.
Back acne, often called bacne, affects roughly 5‑10 % of adolescents and adults alike, yet many people overlook it because it’s hidden from view. Ignoring the problem can lead to scarring, hyperpigmentation, and a loss of confidence. By following evidence‑based steps, you can reduce inflammation, prevent future eruptions, and restore a smooth, healthy back.
In the sections that follow, we’ll cover everything from daily cleansing techniques and the best ingredients—such as bacne benzoyl peroxide—to lifestyle adjustments that support clear skin. You’ll also learn when it’s time to seek specialized care at a dermatology clinic, like Gold City Medical Center, where integrative approaches combine medical expertise with cosmetic precision.
Understanding Bacne: Causes and Triggers
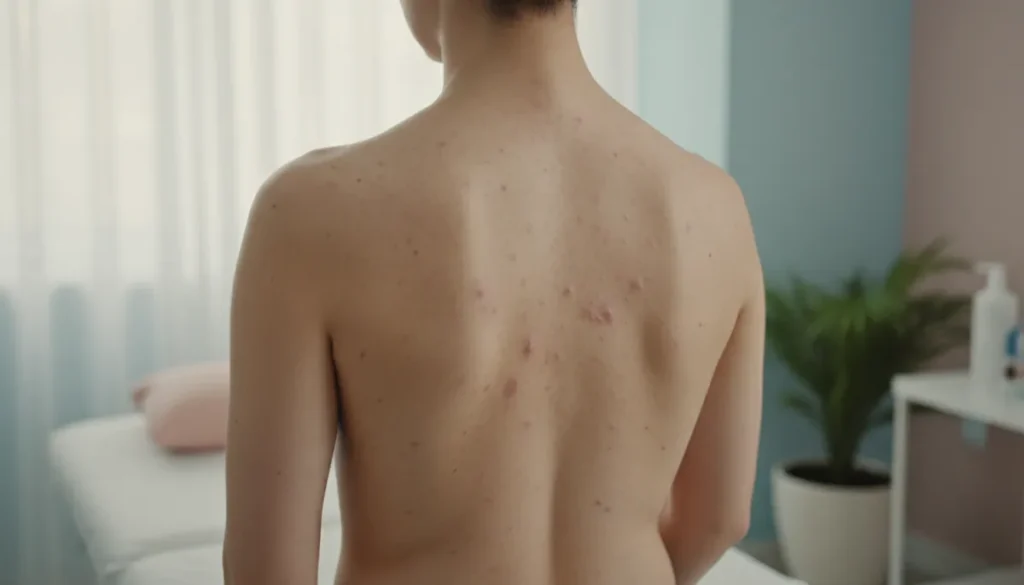
Bacne, or back acne, develops when hair follicles become clogged with excess oil, dead skin cells, and bacteria. Several factors can amplify this process:
- Hormonal fluctuations during puberty, menstrual cycles, or stress increase sebum production.
- Friction from tight clothing, backpacks, or sports equipment creates a micro‑environment that traps sweat and oil.
- Improper hygiene, such as infrequent showering after heavy exercise, leaves the skin vulnerable to bacterial overgrowth.
- Genetic predisposition: a family history of acne can make you more prone to bacne.
- Dietary influences, especially high‑glycemic foods, may exacerbate inflammation.
Understanding these triggers helps you target the root causes rather than just treating surface symptoms. Below is a quick reference that matches common causes with preventive actions:
| Cause | Preventive Action |
|---|---|
| Hormonal spikes | Maintain a balanced diet, manage stress, consider medical advice for hormonal regulation. |
| Friction | Wear loose‑fitting, breathable fabrics; use padded straps for backpacks. |
| Poor hygiene | Shower within 30 minutes after sweating; use a gentle bacne shower gel. |
| Genetics | Adopt a proactive skincare routine early; consult a dermatologist for personalized treatment. |
| Dietary factors | Limit sugary snacks; increase intake of omega‑3 fatty acids and antioxidants. |
Daily Skincare Routine for Bacne
Consistent cleansing is the cornerstone of any bacne‑fighting plan. Below is a step‑by‑step routine that incorporates ingredients proven to reduce breakouts:
- Pre‑shower cleanse: Use a gentle bacne shower gel containing salicylic acid to dissolve excess oil and unclog pores before you even step into the water.
- Warm water rinse: Warm (not hot) water opens pores, allowing the cleanser to work more effectively. Spend 2‑3 minutes gently massaging the back with a soft cleansing brush.
- Targeted treatment: After drying, apply a thin layer of bacne benzoyl peroxide (2.5 %–5 %) to active spots. This helps kill acne‑causing bacteria.
- Moisturize: Choose a non‑comedogenic, oil‑free moisturizer to restore barrier function without feeding the bacteria.
- Sun protection: If you spend time outdoors, use a broad‑spectrum sunscreen formulated for the body to prevent post‑inflammatory hyperpigmentation.
Repeating this routine twice daily—morning and evening—maximizes the benefits of each product and keeps the skin’s microbiome balanced. For those who prefer a more natural approach, a tea‑tree oil solution can serve as an adjunct to benzoyl peroxide, offering antimicrobial action without harsh chemicals.
Targeted Treatments: Over‑the‑Counter and Prescription Options
When lifestyle changes alone aren’t enough, topical and oral medications can accelerate healing. Below is a concise overview of the most common options:
| Type | Active Ingredient | Typical Use | Potential Side Effects |
|---|---|---|---|
| OTC Gel | Benzoyl peroxide (2.5 %–5 %) | Spot‑treat active bacne lesions | Dryness, mild irritation |
| OTC Cleanser | Salicylic acid (0.5 %–2 %) | Daily cleansing to prevent clogged pores | Temporary tingling |
| Prescription Cream | Retinoids (tretinoin, adapalene) | Accelerate cell turnover, reduce inflammation | Redness, peeling |
| Oral Medication | Isotretinoin or oral antibiotics | Severe or cystic bacne unresponsive to topicals | Dry lips, elevated liver enzymes |
For most people, starting with an OTC regimen—such as bacne benzoyl peroxide combined with a salicylic acid cleanser—provides noticeable improvement within 2‑4 weeks. If lesions persist, a dermatologist may prescribe a retinoid or, in more severe cases, isotretinoin. Spot‑treat bacne with a targeted gel, and use a broader body acne treatment (e.g., a medicated body wash) for maintenance.
Lifestyle Changes and Home Remedies
Beyond products, daily habits play a crucial role in preventing bacne flare‑ups. Incorporate these evidence‑based strategies into your routine:
- Exercise wisely: Sweat can aggravate bacne if you remain in tight clothing for long periods. Change into breathable fabrics and shower promptly after workouts.
- Hydration: Drinking at least 2 liters of water daily helps maintain skin elasticity and supports detoxification.
- Dietary balance: Reduce high‑glycemic foods, dairy, and processed snacks. Emphasize leafy greens, lean proteins, and omega‑3 rich foods like salmon.
- Stress management: Chronic stress elevates cortisol, which can increase oil production. Practices such as mindfulness, yoga, or short walks can mitigate this effect.
- Home remedies: A gentle DIY mask of equal parts honey and cinnamon can provide antibacterial benefits. Apply for 10‑15 minutes, then rinse thoroughly.
While home remedies can complement clinical treatments, they are most effective when combined with proper hygiene and targeted products. Consistency is key; visible improvements typically appear after 3‑6 weeks of sustained effort.
When to Seek Professional Care
Most bacne cases respond well to diligent home care, but certain signs indicate that professional intervention is necessary. Seek a dermatologist if you notice any of the following:
- Persistent nodules or cysts that do not improve after 8‑12 weeks of OTC treatment.
- Severe pain, swelling, or signs of infection (e.g., pus, fever).
- Extensive scarring or hyperpigmentation that affects self‑esteem.
- Acne that recurs rapidly after each treatment cycle.
At Gold City Medical Center, our dermatology team offers comprehensive assessments, including skin‑type analysis and, when appropriate, advanced procedures such as chemical peels, laser therapy, and bacne scars treatment. Early professional care can prevent long‑term damage and accelerate the path to smooth, blemish‑free skin.
Why Choose Gold City Medical Center
Gold City Medical Center combines cutting‑edge dermatological expertise with a holistic approach to skin health. Our specialists tailor treatments to each individual, blending medical‑grade options like prescription retinoids with aesthetic procedures that minimize scarring. With state‑of‑the‑art facilities and a commitment to patient‑centered care, we help you achieve lasting results for bacne and overall skin wellbeing.
Ready to clear your back and boost your confidence? Book a consultation with our skin‑care experts today and start your personalized journey toward a smoother, healthier complexion.
Contact Gold City Medical Center now and discover the integrative solutions that work for you.
FAQ
What causes bacne?
Bacne is triggered by hormonal changes, friction, poor hygiene, genetics, and diet.
How can I prevent bacne?
Maintain good hygiene, wear breathable clothing, manage stress, and follow a balanced diet.
What is the best daily skincare routine for bacne?
Cleanse with salicylic acid, apply benzoyl peroxide to spots, moisturize, and protect with sunscreen.
Which over‑the‑counter treatments are effective for bacne?
Benzoyl peroxide gels, salicylic acid cleansers, and retinoid creams are the most common OTC options.
When should I see a dermatologist for bacne?
Seek professional care if lesions persist after 8‑12 weeks of OTC treatment or if you experience pain, cysts, or scarring.
Can diet affect bacne?
Yes, high‑glycemic foods, dairy, and processed snacks can worsen bacne, while omega‑3s and antioxidants help.
What home remedies can help with bacne?
A honey‑cinnamon mask, tea‑tree oil solution, and gentle exfoliation can complement medical treatments.