Finding a reliable kp skin cure can feel overwhelming when you’re dealing with persistent bumps and redness on your arms, legs, or face. This article explains what causes keratosis pilaris, outlines practical self‑care steps, and reviews professional options available at Gold City Medical Center. With up to 9,900 monthly searches, many people are seeking clear answers to manage this common skin condition.
Keratosis pilaris, often called “chicken skin,” appears as tiny, rough bumps that may be red, pink, or skin‑colored. While harmless, it can affect confidence and comfort, especially when the bumps become itchy or inflamed. Understanding the underlying mechanisms is the first step toward an effective cure.
In the sections below, you’ll discover evidence‑based strategies, from moisturizers and exfoliators to laser and chemical peel treatments. Whether you prefer a DIY regimen or a clinical approach, we provide actionable guidance to help you achieve smoother, healthier skin.
Understanding Keratosis Pilaris: Causes and Symptoms
Keratosis pilaris (KP) is a genetic skin disorder characterized by the buildup of keratin around hair follicles, forming tiny plugs that create a rough texture. The condition often appears during adolescence and may persist into adulthood.
Key factors that contribute to KP include:
- Genetic predisposition – a family history of “chicken skin” increases likelihood.
- Dry skin – low moisture levels exacerbate keratin buildup.
- Hormonal changes – puberty, pregnancy, or menopause can trigger flare‑ups.
- Environmental factors – cold, low‑humidity climates worsen symptoms.
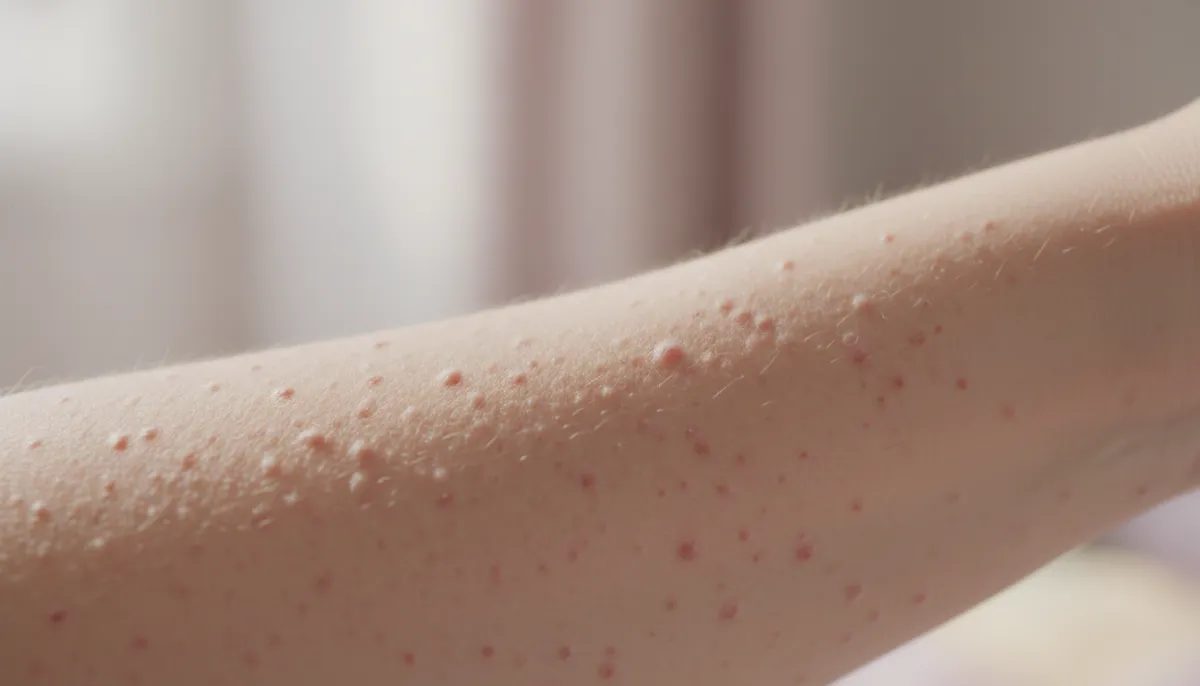
Typical symptoms encompass small bumps on skin, especially on the upper arms, thighs, cheeks, and buttocks. Some individuals notice red bumps on skin or experience occasional itching, described as “tiny itchy bumps on skin.” While the bumps are generally painless, they can become inflamed, leading to a “rash on arms” or “red spots on arms.”
Because KP is a keratinization disorder, it is not an infection and does not require antibiotics. However, the visible texture often prompts people to seek a kp skin cure through both topical and procedural treatments.
Daily Skincare Routine for Managing KP
A consistent daily regimen is the cornerstone of any kp skin cure. While no single product eliminates the condition, the right combination of moisturizers, exfoliators, and gentle cleansers can dramatically improve texture and reduce redness.
Step 1: Gentle Cleansing
Choose a fragrance‑free, sulfate‑free cleanser to avoid stripping natural oils. Cleansing twice daily helps remove dead skin cells without irritating the follicles.
Step 2: Exfoliation
Incorporate a mild chemical exfoliant 2–3 times per week. Products containing alpha‑hydroxy acids (AHA) or beta‑hydroxy acids (BHA) dissolve keratin plugs and smooth the surface. Avoid harsh physical scrubs, which can aggravate “tiny colorless itchy bumps on skin.”
Step 3: Moisturizing
After cleansing, apply a thick, fragrance‑free moisturizer for kp that contains ceramides, urea, or lactic acid. These ingredients restore the skin barrier and attract water to the epidermis, reducing “chicken skin” appearance.
- Best keratosis pilaris moisturizer options:
- Ceramide‑rich creams (e.g., CeraVe Moisturizing Cream)
- Urea‑based lotions (e.g., Eucerin Roughness Relief)
- Lactic acid creams (e.g., AmLactin Daily Moisturizing Body Lotion)
Step 4: Sun Protection
Daily sunscreen (SPF 30 or higher) prevents further skin barrier damage and minimizes hyperpigmentation that can follow inflammation.
Adhering to this routine can significantly lessen the visibility of “bumps on arms” and “small red bumps on the skin,” providing a solid foundation for any kp skin cure plan.
Professional Treatments Available
When at‑home care does not achieve the desired results, professional keratosis pilaris treatment options can accelerate improvement. Gold City Medical Center offers several evidence‑based procedures tailored to individual skin types and severity.
Laser Therapy
Fractional lasers target the excess keratin and stimulate collagen production, smoothing the skin’s surface. Multiple sessions are typically required, with minimal downtime.
Chemical Peels
Medium‑strength peels containing glycolic or trichloroacetic acid (TCA) can dissolve keratin plugs and promote cell turnover. Peels are performed by licensed dermatologists and are suitable for larger areas such as thighs and buttocks.
Microdermabrasion
This mechanical exfoliation method gently sands the outer skin layer, reducing the appearance of “tiny itchy bumps on legs” and improving overall texture.
| Treatment | How It Works | Number of Sessions | Typical Downtime |
|---|---|---|---|
| Laser Therapy | Targets keratin plugs with focused light | 3–5 | 1–2 days redness |
| Chemical Peel | Exfoliates with glycolic/TCA acids | 2–4 | 3–5 days flaking |
| Microdermabrasion | Mechanical sanding of epidermis | 4–6 | Same‑day mild erythema |
Each of these kp disease treatment modalities is performed under strict medical supervision to ensure safety and optimal outcomes. Discussing your skin history with a specialist will determine the most appropriate approach for your kp skin cure journey.
Lifestyle Tips to Prevent Flare‑Ups
Even with effective treatments, lifestyle choices play a crucial role in maintaining smooth skin and preventing new “bumps on legs that look like pimples.”
- Hydration: Drink at least 8 glasses of water daily to keep the epidermis hydrated from within.
- Humidity Control: Use a humidifier in dry indoor environments, especially during winter.
- Clothing Choices: Opt for breathable, natural fabrics (cotton, bamboo) to reduce friction that can irritate follicles.
- Gentle Exercise: Regular low‑impact activities improve circulation without excessive sweating that may aggravate “itchy spots arms.”
- Dietary Considerations: Incorporate omega‑3 fatty acids (fish, flaxseed) and antioxidants (berries, leafy greens) to support skin health.
Avoiding harsh soaps, hot showers, and prolonged exposure to cold, dry air can also minimize “keratosis pilaris causes” linked to barrier disruption. By integrating these habits, you reinforce the benefits of any medical or topical kp skin cure you pursue.
When to Seek Medical Advice
Most cases of keratosis pilaris are benign, but certain signs indicate the need for professional evaluation. Seek a dermatologist if you notice:
- Persistent inflammation or swelling that does not improve with moisturizers.
- Severe itching accompanied by “red itchy pimples on legs” or “rash on arms.”
- Signs of infection, such as pus, warmth, or spreading redness.
- Sudden changes in the color or size of the bumps, especially darkening (possible post‑inflammatory hyperpigmentation).
Gold City Medical Center’s dermatology team can perform a thorough assessment, rule out other conditions (e.g., eczema or folliculitis), and design a personalized treatment plan. Early intervention often leads to faster, more lasting results for your kp skin cure goals.
Why Choose Gold City Medical Center
Gold City Medical Center combines integrative medicine with advanced cosmetic expertise, offering a holistic approach to skin health. Our board‑certified dermatologists tailor each keratosis pilaris treatment to the individual, ensuring safety, comfort, and effective outcomes. With state‑of‑the‑art laser technology and a commitment to evidence‑based care, we help patients achieve smoother, healthier skin while maintaining overall wellbeing.
Ready to start your kp skin cure journey? Contact Gold City Medical Center today to schedule a personalized skin assessment and discover the treatment plan that’s right for you.
Call now or fill out our online request form—smooth, confident skin is just a step away.
FAQ
What causes keratosis pilaris and how can I identify its symptoms?
Keratosis pilaris is caused by a genetic tendency to produce excess keratin that blocks hair follicles, often worsened by dry skin, hormonal changes, and cold climates. Symptoms include tiny rough bumps on the arms, thighs, cheeks, or buttocks, sometimes accompanied by redness or itching.
What daily skincare routine steps are recommended for managing keratosis pilaris?
A recommended routine includes gentle cleansing, 2–3 times weekly chemical exfoliation with AHA or BHA, daily moisturization with ceramide‑rich or urea‑based creams, and sunscreen use.
Which exfoliants are effective for reducing KP bumps?
Mild chemical exfoliants containing AHAs (like glycolic acid) or BHAs (like salicylic acid) are most effective, while physical scrubs should be avoided.
What professional treatments does Gold City Medical Center offer for keratosis pilaris?
Gold City Medical Center provides laser therapy, chemical peels, and microdermabrasion, each designed to target keratin buildup and improve skin texture.
When should I seek medical advice for keratosis pilaris?
Seek a dermatologist if you experience persistent inflammation, severe itching, signs of infection, or sudden changes in bump color or size.
How does laser therapy improve keratosis pilaris skin texture?
Laser therapy targets keratin plugs with focused light, breaking them down and stimulating collagen to smooth the skin.
What lifestyle habits can help prevent KP flare‑ups?
Staying hydrated, using a humidifier, wearing breathable fabrics, gentle exercise, and a diet rich in omega‑3s and antioxidants can reduce flare‑ups.