Many people notice keratosis pilaris face symptoms and wonder why smooth skin suddenly looks rough and bumpy. This common skin condition, often called “chicken skin,” can appear on the cheeks, forehead, or chin, creating tiny red or skin‑colored bumps that may be itchy or uncomfortable. Although harmless, the visual impact can affect confidence, especially when the face is involved.
In this article we will explore what causes keratosis pilaris on the face, how to recognize its signs, and which evidence‑based treatments and daily habits can improve the texture and appearance of the skin. Whether you are seeking over‑the‑counter moisturizers, professional medical procedures, or simple lifestyle adjustments, the information here is designed to guide you toward clearer, smoother skin.
According to dermatology studies, up to 20 % of adolescents experience facial KP at some point, making it one of the most frequent cosmetic concerns in young adults. Understanding the underlying mechanisms helps you choose the right approach rather than relying on trial‑and‑error solutions.
Read on to discover practical steps, treatment options available at Gold City Medical Center, and long‑term strategies to keep your skin looking its best.
What Is Keratosis Pilaris on the Face?
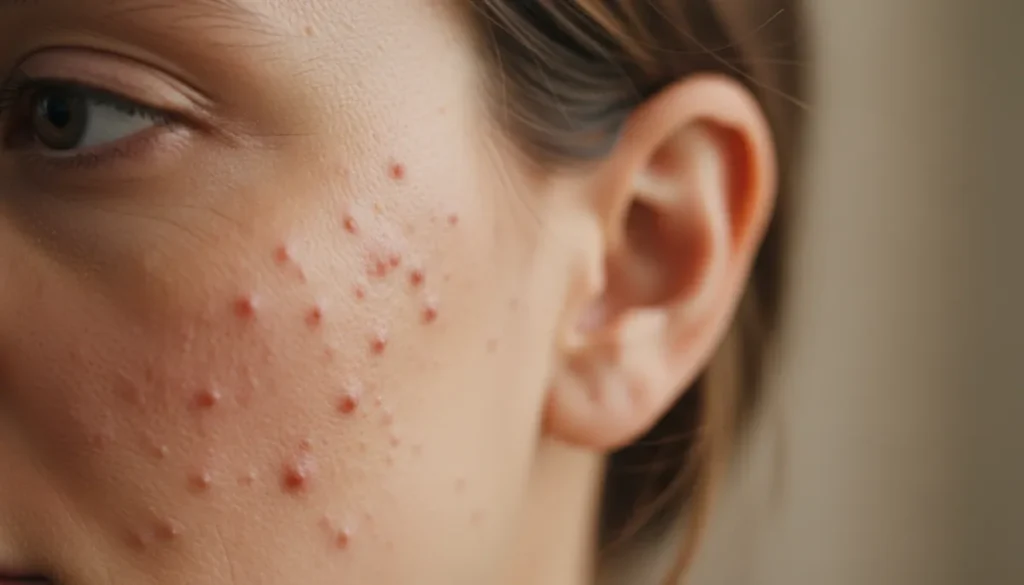
Keratosis pilaris (KP) is a genetic skin disorder characterized by the buildup of keratin—a protein that protects skin—from blocking hair follicles. When this occurs on the face, the result is a pattern of tiny, rough papules that may appear as “red bumps on skin” or “little bumps on skin.” While the exact cause is not fully understood, factors such as dry skin, hormonal changes, and a family history of KP increase the likelihood of developing the condition.
Typical symptoms include:
- Small, flesh‑colored or reddish bumps, often resembling goosebumps.
- Itching or mild irritation, especially after exposure to cold or dry air.
- Visible texture changes on the cheeks, jawline, or forehead.
KP is not dangerous, but its appearance can be distressing. The condition often co‑exists with other skin issues like eczema or acne, which can complicate treatment decisions. Recognizing the difference between “strawberry skin” (KP) and acne lesions is essential for selecting appropriate products.
Below is a quick comparison of common facial skin concerns to help you identify keratosis pilaris:
| Feature | Keratosis Pilaris | Acne | Eczema |
|---|---|---|---|
| Bump size | 1–3 mm, uniform | Variable, can be larger | Often larger, inflamed |
| Color | Skin‑colored to reddish | Red, sometimes pus‑filled | Red, dry patches |
| Location | Cheeks, forehead, jawline | Throughout face, especially T‑zone | Flexural areas, can affect face |
| Itchiness | Mild to moderate | Variable | Common |
Building an Effective Skincare Routine for Facial KP
Consistent daily care is the cornerstone of managing keratosis pilaris on the face. A routine that combines gentle cleansing, targeted exfoliation, and deep moisturization can reduce the appearance of bumps and soothe irritation.
Cleansing
Choose a mild, sulfate‑free cleanser that removes excess oil without stripping the skin’s natural barrier. Look for ingredients such as glycerin or panthenol, which help retain moisture. Cleansing twice daily—morning and night—prepares the skin for subsequent treatment steps.
Exfoliation
Exfoliation helps dissolve the keratin plugs that cause bumps. Chemical exfoliants are generally preferred over physical scrubs because they are less abrasive. Effective options include:
- Lactic acid (5–10 %): gentle alpha‑hydroxy acid (AHA) that smooths texture.
- Glycolic acid (5 %): stronger AHA for more pronounced resurfacing.
- Salicylic acid (0.5–2 %): beta‑hydroxy acid (BHA) that penetrates pores and reduces inflammation.
Introduce an exfoliant 2–3 times per week, gradually increasing frequency based on tolerance. Over‑exfoliation can worsen dryness and cause redness, so monitor your skin’s response.
Moisturizing
After exfoliation, lock in hydration with a moisturizer that contains ceramides, urea, or hyaluronic acid. These ingredients restore the skin barrier and soften the keratin buildup. Popular “moisturizers for kp” include:
- Ceramide‑rich creams (e.g., CeraVe Moisturizing Cream).
- Urea‑based lotions (10 % urea for intensive smoothing).
- Oil‑free gel moisturizers with hyaluronic acid for oily skin types.
Apply moisturizer while the skin is still damp to seal in moisture effectively. Consistency is key; daily use can lead to noticeable improvement within 4–6 weeks.
Professional Medical Treatments for Facial KP
When over‑the‑counter methods do not provide sufficient results, medical interventions can accelerate improvement. Gold City Medical Center offers several evidence‑based treatments tailored to the delicate facial area.
Laser Therapy
Fractional laser resurfacing targets the thickened keratin plugs without damaging surrounding tissue. The procedure stimulates collagen production, leading to smoother skin and reduced redness. Most patients require 2–4 sessions spaced four weeks apart.
Chemical Peels
Professional chemical peels using trichloroacetic acid (TCA) or a combination of AHAs can effectively exfoliate deeper layers of the epidermis. Peels are performed by a dermatologist and are followed by a short recovery period during which moisturization is essential.
Prescription Topicals
For persistent cases, dermatologists may prescribe topical retinoids (e.g., tretinoin) or combination creams containing urea and lactic acid. These formulations work by normalizing keratinocyte turnover and reducing follicular plugging.
Below is a summary of the most common medical options:
| Treatment | Mechanism | Number of Sessions | Typical Downtime |
|---|---|---|---|
| Fractional Laser | Micro‑thermal zones remodel skin | 2–4 | 1–3 days redness |
| Chemical Peel (TCA) | Controlled epidermal exfoliation | 1–3 | 3–5 days flaking |
| Prescription Retinoid | Regulates keratinization | Ongoing | Minimal, possible irritation |
All procedures are performed under sterile conditions, and a personalized after‑care plan is provided to maximize results while minimizing side effects.
Lifestyle Adjustments and Home Remedies
Beyond products and procedures, everyday habits influence the severity of keratosis pilaris on the face. Simple changes can complement medical treatment and help maintain results.
Hydration and Diet
Staying well‑hydrated supports skin elasticity. Aim for at least eight glasses of water daily. A diet rich in omega‑3 fatty acids (found in fish, flaxseed, and walnuts) can reduce inflammation, while limiting excessive sugar and processed foods helps prevent flare‑ups.
Environmental Factors
Dry indoor air, especially during winter, can exacerbate KP. Using a humidifier adds moisture to the environment, reducing skin dryness. Additionally, protect your face from harsh wind and cold by applying a barrier cream before going outdoors.
Clothing and Grooming
Although facial KP is not directly caused by clothing, avoiding rough fabrics that may irritate the skin (e.g., wool scarves) can prevent secondary inflammation. When shaving or using facial hair removal tools, opt for a gentle, fragrance‑free shave gel and replace blades regularly.
Key home‑care tips summarized:
- Apply a fragrance‑free moisturizer immediately after washing.
- Use a humidifier in dry rooms.
- Incorporate omega‑3 rich foods and limit sugary snacks.
- Choose soft, breathable fabrics for facial coverings.
- Perform gentle chemical exfoliation 2–3 times weekly.
Managing Expectations and Long‑Term Care
Keratosis pilaris is a chronic condition, meaning that while symptoms can be significantly reduced, they may recur if maintenance is neglected. Understanding realistic outcomes helps you stay motivated and avoid disappointment.
Progress Timeline
Most patients notice smoother skin within 4–8 weeks of consistent routine, but full clearance can take several months. Patience is essential; abrupt changes in product usage often lead to temporary worsening.
When to Seek Professional Help
If you experience persistent redness, swelling, or pain, or if over‑the‑counter moisturizers and exfoliants do not improve the texture after three months, schedule a consultation. Early intervention with laser or prescription therapy can prevent deeper keratin buildup.
Maintenance Strategy
Even after achieving desired results, continue a simplified regimen:
- Gentle cleanser twice daily.
- Low‑strength AHA serum 2–3 times per week.
- Ceramide‑rich moisturizer daily.
- Periodic professional check‑ups every 6–12 months.
Adhering to this plan helps keep the skin barrier strong and minimizes the likelihood of flare‑ups.
Why Choose Gold City Medical Center
Gold City Medical Center combines integrative medicine with cutting‑edge cosmetic expertise, offering personalized solutions for keratosis pilaris on the face. Our multidisciplinary team evaluates each patient’s skin type, lifestyle, and goals to create a tailored treatment plan that may include laser therapy, professional peels, or prescription topicals. With a focus on safety, efficacy, and patient comfort, we ensure you receive the most appropriate care in a welcoming environment.
Ready to smooth your skin and regain confidence? Contact Gold City Medical Center today to schedule a personalized skin assessment and discover the best treatment pathway for your facial keratosis pilaris.
FAQ
What causes keratosis pilaris on the face?
Keratosis pilaris on the face is caused by a buildup of keratin that blocks hair follicles, often worsened by dry skin, hormonal changes, and genetics.
How can I tell if my facial bumps are keratosis pilaris or acne?
KP bumps are uniform, flesh‑colored or reddish, often non‑inflamed, whereas acne lesions vary in size, can contain pus, and are usually more inflamed.
What are the best over‑the‑counter products for facial KP?
Gentle sulfate‑free cleansers, chemical exfoliants containing lactic, glycolic, or salicylic acid, and moisturizers rich in ceramides, urea, or hyaluronic acid work best.
Are laser therapy and chemical peels effective for treating facial keratosis pilaris?
Yes, both fractional laser resurfacing and professional chemical peels can significantly improve texture and redness when performed by a dermatologist.
How long does it take to see improvement with a skincare routine for KP?
Most patients notice smoother skin within 4–8 weeks, but full clearance can take several months of consistent use.
What lifestyle changes can help reduce facial keratosis pilaris?
Staying hydrated, eating omega‑3‑rich foods, using a humidifier in dry environments, and avoiding harsh fabrics or irritants support smoother skin.





