The early signs of a receding hairline often appear subtly, yet recognizing them promptly can make a significant difference in long‑term hair health. Many individuals notice a slight widening at the temples or a gradual thinning along the frontal edge, but they may dismiss these changes as normal aging. In reality, these initial indicators can signal underlying processes such as androgenetic alopecia or other forms of alopecia. According to recent dermatological surveys, roughly 30 % of men and 10 % of women notice noticeable hairline recession before the age of 30, highlighting the importance of early detection.
This article explains what to look for, why these changes occur, and how you can act before the hair loss progresses. By understanding the underlying mechanisms, you’ll be better equipped to choose appropriate treatments, whether they involve lifestyle adjustments, medical therapies, or advanced hair‑restoration procedures.
We will explore the science behind hairline recession, identify the most common early indicators, discuss when professional evaluation is advisable, and outline practical strategies to preserve your hair density. Let’s begin by demystifying the causes that drive the hairline to move backward.
Understanding Hairline Recession: Causes and Mechanisms
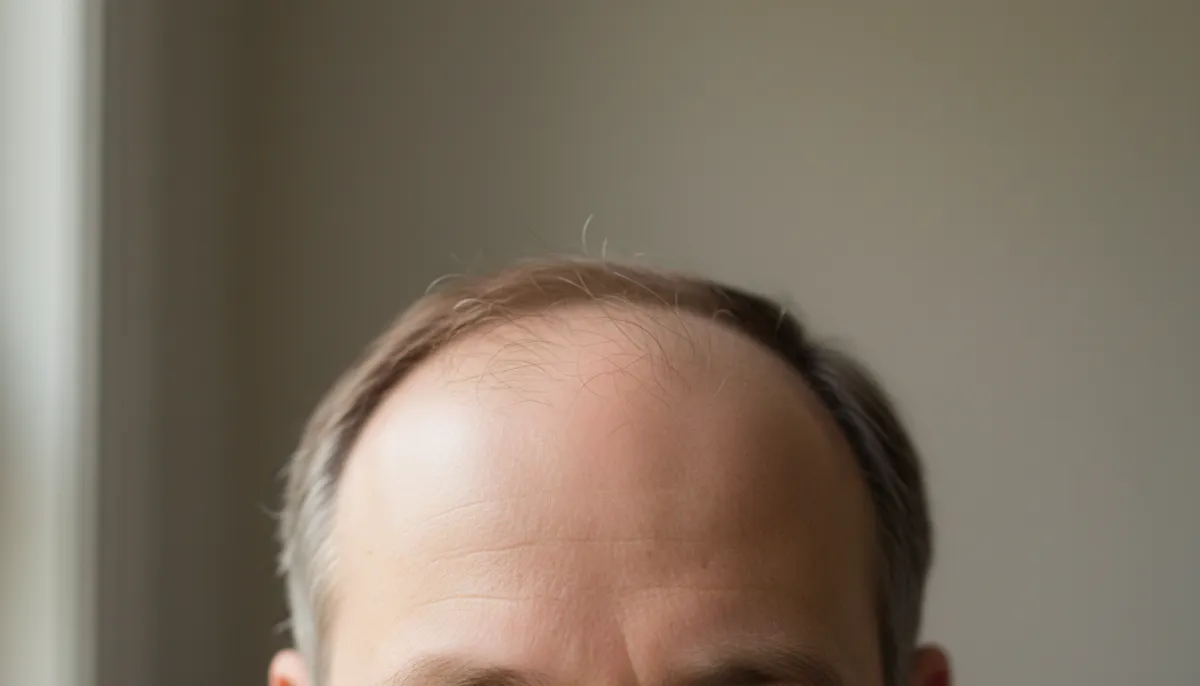
Hairline recession does not happen overnight; it is the result of a complex interplay between genetics, hormones, and environmental factors. The most common driver is androgenetic alopecia, often referred to as male or female pattern baldness. In this condition, dihydrotestosterone (DHT) binds to hair follicles, shortening the growth phase and causing follicles to miniaturize. Over time, the affected area becomes progressively thinner, creating the classic “M‑shaped” pattern in men and a diffuse thinning along the front in women.
Other contributors include:
- Genetic predisposition – family history strongly influences susceptibility.
- Hormonal fluctuations – especially elevated DHT levels.
- Traction alopecia – chronic pulling from tight hairstyles.
- Autoimmune reactions – such as alopecia areata, which can cause sudden patchy loss.
- Medical conditions and medications – thyroid disorders, chemotherapy, and certain antidepressants.
Below is a comparison of the primary causes and their typical presentation:
| Cause | Typical Pattern | Age of Onset |
|---|---|---|
| Androgenetic alopecia | M‑shaped recession, vertex thinning | Late teens to 40s |
| Traction alopecia | Frontal or temporal thinning, often symmetrical | Any age, linked to hairstyle |
| Alopecia areata | Sudden, well‑defined patches | Variable, can affect any age |
| Medical‑induced loss | Diffuse thinning, sometimes rapid | During treatment period |
Understanding which factor is at play is essential for selecting the most effective intervention. While genetics cannot be changed, many of the other contributors are modifiable through lifestyle choices and targeted therapies.
Key Early Indicators to Watch For
Spotting the first signs of a receding hairline empowers you to act before the condition advances. The most reliable early indicators include:
- Temple thinning – a gradual loss of density at the sides of the forehead, often creating a subtle “M” shape.
- Increased hair shedding during washing or brushing – more than 100 hairs per day may be a warning sign.
- Visible “bald spot” at the hairline – small, often circular areas where hair appears thinner.
- Changes in hair texture – fine, soft hair replaces the previously thicker strands.
- Family history confirmation – if close relatives experienced early hairline recession, your risk is higher.
These symptoms are frequently accompanied by broader hair thinning across the scalp, especially in individuals with male pattern baldness. Women may notice a widening of the part line or a general reduction in volume rather than a distinct recession.
Regular self‑examination is simple: part your hair in the middle and observe the density at the temples and along the frontal edge. Taking photos every few weeks can help you detect subtle changes that are otherwise easy to miss.
When to Seek Professional Evaluation
If you notice any of the early signs described above, it is advisable to schedule a consultation with a qualified specialist. Early professional evaluation can differentiate between benign thinning and more serious conditions such as alopecia areata or underlying hormonal imbalances.
During the appointment, clinicians typically perform:
- A detailed medical history to uncover potential triggers.
- Scalp examination, often aided by a trichoscope for magnified visualization.
- Blood tests to assess hormone levels, iron, thyroid function, and other markers.
- Possibly a scalp biopsy if an autoimmune disorder is suspected.
The following table outlines common symptoms and the recommended next steps:
| Symptom | Possible Cause | Recommended Action |
|---|---|---|
| Gradual temple thinning | Androgenetic alopecia | Consult dermatologist; consider DHT‑blocking treatment. |
| Sudden patchy loss | Alopecia areata | Dermatology referral; evaluate for autoimmune therapy. |
| Hair loss linked to tight hairstyles | Traction alopecia | Modify styling; seek professional advice if persistent. |
| Excessive shedding during medication | Drug‑induced alopecia | Discuss alternatives with prescribing physician. |
Prompt evaluation not only clarifies the diagnosis but also opens the door to early‑stage treatments that are more effective when the hair follicles are still viable.
Effective Prevention and Early Intervention Strategies
Once a diagnosis is confirmed, a combination of lifestyle adjustments and medical interventions can halt or even reverse early hairline recession. Below are proven strategies that address the root causes:
Topical and Oral Medications
- Minoxidil – a vasodilator that prolongs the growth phase of hair follicles; available over‑the‑counter in 2 % and 5 % formulations.
- Finasteride or Dutasteride – oral DHT blockers prescribed for men; they reduce the hormone’s impact on follicles.
- Spironolactone – an anti‑androgen used off‑label for women with hormonal‑related thinning.
Procedural Options
- Platelet‑Rich Plasma (PRP) therapy – concentrates growth factors from your own blood to stimulate follicular activity.
- Low‑Level Laser Therapy (LLLT) – non‑invasive light treatment that improves cellular metabolism in the scalp.
- Hair transplantation – Follicular Unit Extraction (FUE) or Follicular Unit Transplantation (FUT) for permanent restoration when the recession has progressed.
Lifestyle and Nutritional Support
- Balanced diet rich in iron, zinc, biotin, and omega‑3 fatty acids.
- Avoiding excessive heat styling, tight hairstyles, and harsh chemical treatments.
- Stress management through regular exercise, meditation, or counseling.
Combining these approaches often yields the best results. For example, a patient might use minoxidil daily while undergoing PRP sessions every three months, complemented by a diet optimized for hair health.
Monitoring Progress and Adjusting Treatment Plans
Consistent monitoring is crucial to determine whether a chosen regimen is effective. Most clinicians recommend a structured follow‑up schedule:
- Baseline photos and hair density measurements at the start of treatment.
- Quarterly assessments for the first year to track changes.
- Adjustment of medication dosage or addition of procedures based on observed response.
Digital tools, such as trichoscopy apps, can quantify hair count and thickness, providing objective data to guide decisions. If progress stalls, a switch to an alternative therapy—like adding oral finasteride to a topical regimen—may be warranted.
Remember that early intervention offers the highest probability of preserving existing follicles. Patience and adherence to the treatment plan are essential, as visible improvement often takes 3‑6 months to become apparent.
Why Choose Gold City Medical Center
Gold City Medical Center combines cutting‑edge medical expertise with a holistic approach to hair health. Our team of experienced dermatologists and hair‑restoration surgeons offers personalized assessments, state‑of‑the‑art diagnostics, and a full spectrum of treatments—from topical solutions to advanced FUE transplantation. We prioritize patient comfort, evidence‑based outcomes, and seamless integration of aesthetic and medical care, ensuring you receive the most effective solution for your early hairline concerns.
Ready to protect your hair before the recession becomes noticeable? Contact Gold City Medical Center today to schedule a comprehensive scalp evaluation and receive a tailored prevention plan.
Take the first step toward lasting confidence—call now or fill out our online consultation form.
FAQ
What are the first signs that my hairline is receding?
Early signs include temple thinning, increased shedding, a small bald spot at the hairline, changes in hair texture, and a family history of early recession.
How does androgenetic alopecia cause a receding hairline?
Androgenetic alopecia involves DHT binding to hair follicles, shortening the growth phase and causing miniaturization, which leads to a receding hairline.
When should I see a dermatologist for hair loss?
If you notice any early signs like temple thinning, sudden patches, or excessive shedding, schedule a dermatologist visit promptly.
What non‑prescription treatments help prevent hairline recession?
Topical minoxidil, balanced nutrition, stress management, and gentle hair‑care practices are effective non‑prescription options.
How long does it take to see results from hair loss treatments?
Visible improvement typically appears after 3–6 months of consistent treatment, though individual response varies.
What advanced procedures are available for early hairline recession?
Procedures include PRP therapy, low‑level laser therapy, and hair transplantation (FUE or FUT) for more advanced cases.





