Scalp eczema is a common inflammatory skin condition that affects the scalp, causing itching, redness, and flaking. It can be confusing because its signs often resemble dandruff or seborrheic dermatitis, leading many to overlook the underlying issue. Recognizing the condition early is crucial for preventing discomfort and potential hair loss.
In this article we explore what scalp eczema is, why it appears, and how you can manage it effectively. Whether you are dealing with occasional itchiness or persistent flare‑ups, understanding the root causes empowers you to choose the right treatment plan.
Recent studies indicate that up to 10 % of adults experience some form of scalp eczema during their lifetime, making it one of the most frequent dermatological concerns in modern clinics. This prevalence underscores the importance of accurate diagnosis and tailored therapy.
We will walk you through the distinguishing features of scalp eczema, common triggers, symptom recognition, and both medical and at‑home treatment strategies. By the end, you’ll have a clear roadmap to soothe your scalp and restore healthy hair growth.
What Is Scalp Eczema and How Does It Differ From Other Scalp Conditions?
Scalp eczema is a type of dermatitis that specifically targets the skin on the head. Unlike ordinary dandruff, which is primarily caused by excess oil and a yeast called Malassezia, eczema involves an immune‑mediated inflammation that can lead to intense itching and raw patches.
Key differences between scalp eczema and related conditions:
- Eczema vs. Seborrheic Dermatitis: Seborrheic dermatitis often presents with oily, yellowish scales, while eczema tends to be drier and more inflamed.
- Eczema vs. Atopic Dermatitis: Atopic dermatitis is a broader, systemic condition that can affect many body areas; when it appears on the scalp, it is still classified as scalp eczema.
- Eczema vs. Dandruff: Dandruff is usually non‑painful and does not cause redness or swelling, whereas eczema does.
| Condition | Primary Symptoms | Typical Triggers |
|---|---|---|
| Scalp Eczema | Itchy, red patches; dry flakes; possible oozing | Allergens, stress, dry weather |
| Seborrheic Dermatitis | Greasy yellow scales; mild itching | Malassezia overgrowth, hormonal changes |
| Dandruff | White flakes; mild itch | Excess oil, yeast proliferation |
Understanding these nuances helps clinicians choose the most effective therapy and prevents unnecessary use of harsh anti‑dandruff shampoos that may aggravate eczema.
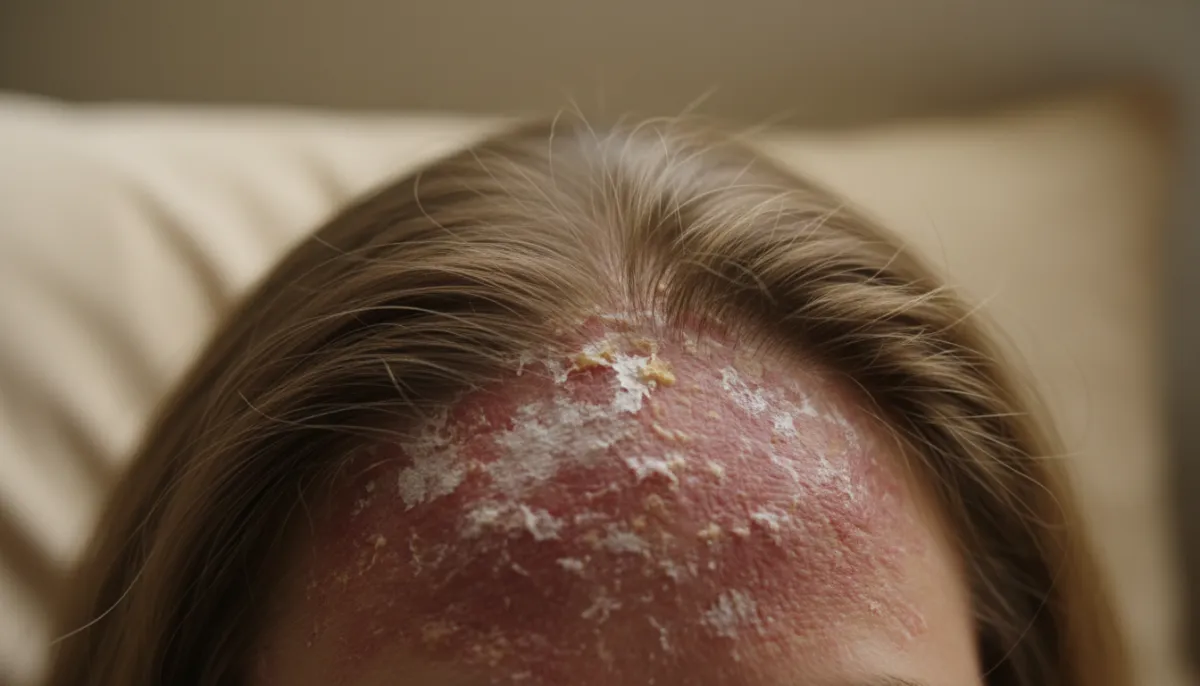
Common Triggers and Underlying Causes of Scalp Eczema
Identifying what sparks a flare‑up is essential for long‑term control. While the exact cause of scalp eczema varies among individuals, several well‑documented triggers are repeatedly reported in clinical practice.
Genetic and Immune Factors
People with a family history of atopic conditions—such as asthma, allergic rhinitis, or eczema on other body parts—are more prone to develop scalp eczema. The immune system in these individuals overreacts to minor irritants, leading to chronic inflammation.
Environmental Influences
- Dry, cold climates that strip moisture from the skin.
- Exposure to harsh chemicals in hair dyes, styling gels, or strong shampoos.
- Frequent use of heat styling tools that damage the scalp barrier.
Allergens and Irritants
Common allergens include fragrances, preservatives, and certain metals found in hair accessories. Even seemingly benign products like scented conditioners can provoke a reaction.
Other notable triggers:
- Stress – cortisol spikes can exacerbate inflammation.
- Hormonal fluctuations – especially during pregnancy or menopause.
- Skin infections – bacterial or fungal overgrowth may worsen eczema.
By keeping a symptom diary, patients can pinpoint which of these factors correlate with their flare‑ups, enabling targeted avoidance strategies.
Recognizing the Symptoms and When to Seek Professional Help
Early detection of scalp eczema can prevent complications such as secondary infection or hair loss. The condition typically follows a recognizable pattern, though severity can differ.
Primary Symptoms
- Intense itching, often described as a crawling sensation.
- Red, inflamed patches that may become scaly or crusty.
- Dry flakes that resemble dandruff but are larger and more persistent.
- Occasional oozing or crust formation after scratching.
Warning Signs Requiring Medical Attention
If you notice any of the following, schedule an appointment with a dermatologist or a specialist at Gold City Medical Center:
- Rapid hair loss localized to affected areas.
- Signs of infection: increasing pain, warmth, pus, or foul odor.
- Persistent symptoms despite over‑the‑counter treatments for more than two weeks.
- Severe redness spreading beyond the scalp to the neck or face.
Professional evaluation typically includes a visual inspection, possible skin scraping, and a review of personal and family medical history. In some cases, a patch test may be performed to identify specific allergens.
Effective Treatment Options and Home Care Strategies
Managing scalp eczema often requires a combination of prescription medications and daily scalp care routines. The goal is to reduce inflammation, restore the skin barrier, and relieve itching.
Medical Therapies
- Topical corticosteroids: Low‑potency steroids for mild cases; higher potency for acute flare‑ups.
- Calcineurin inhibitors: Non‑steroidal options such as tacrolimus ointment, useful for sensitive skin.
- Antifungal shampoos: Useful when seborrheic dermatitis overlaps with eczema.
- Systemic treatments: In severe cases, oral antihistamines or short courses of oral steroids may be prescribed.
Home Care and Over‑the‑Counter Solutions
Complement medical treatment with gentle, consistent scalp hygiene:
| Product Type | Key Benefits | Recommended Use |
|---|---|---|
| Moisturizing shampoo (sulfate‑free) | Reduces dryness, maintains barrier | 2–3 times weekly |
| Medicated scalp rinse (zinc pyrithione) | Controls yeast, soothes inflammation | Once weekly |
| Leave‑in scalp oil (jojoba or almond) | Provides lasting hydration | Apply after washing |
Additional tips:
- Avoid hot water; use lukewarm rinses to prevent further drying.
- Pat the scalp dry with a soft towel—do not rub.
- Limit the use of styling products that contain alcohol or strong fragrances.
Consistency is key; most patients notice improvement within 2–4 weeks of adhering to a tailored regimen.
Preventive Measures and Long‑Term Management
Even after symptoms subside, maintaining scalp health is essential to prevent recurrence of scalp eczema. Prevention focuses on protecting the skin barrier and minimizing exposure to known irritants.
Lifestyle Adjustments
- Stay hydrated: Adequate water intake supports overall skin moisture.
- Balanced diet: Omega‑3 fatty acids, found in fish and flaxseed, help reduce inflammation.
- Stress management: Practices such as yoga, meditation, or regular exercise can lower cortisol levels.
Scalp Care Routine
Adopt a gentle, consistent routine that includes:
- Using a mild, fragrance‑free shampoo no more than twice a week.
- Applying a lightweight, hypoallergenic scalp moisturizer after washing.
- Protecting the scalp from extreme temperatures—wear a hat in cold weather and avoid excessive heat styling.
Regular follow‑up appointments at Gold City Medical Center allow clinicians to adjust treatment plans as needed and monitor for any signs of secondary infection or worsening of the condition.
Why Choose Gold City Medical Center
Gold City Medical Center combines integrative medicine with cutting‑edge dermatological expertise to deliver personalized care for scalp eczema. Our multidisciplinary team evaluates each patient’s unique skin profile, lifestyle, and medical history to design a comprehensive treatment plan. With state‑of‑the‑art facilities and a commitment to ongoing research, we ensure safe, effective solutions that restore comfort and confidence.
Ready to relieve your scalp eczema and regain a healthy scalp? Contact Gold City Medical Center today to schedule a personalized consultation. Experience expert care that puts your comfort first.
FAQ
What are the main symptoms of scalp eczema?
Scalp eczema typically causes intense itching, red inflamed patches, dry flaky scales, and sometimes oozing or crusting after scratching.
How does scalp eczema differ from dandruff and seborrheic dermatitis?
Scalp eczema is an immune‑mediated inflammation with dry, itchy patches, whereas dandruff is a non‑painful, oily flake condition and seborrheic dermatitis presents with greasy yellow scales.
What common triggers can cause scalp eczema flare‑ups?
Triggers include genetic predisposition, dry cold weather, harsh hair chemicals, heat styling tools, fragrances, preservatives, stress, hormonal changes, and skin infections.
When should I see a dermatologist for scalp eczema?
Seek professional help if you experience rapid hair loss, signs of infection, persistent symptoms despite OTC treatment, or spreading redness beyond the scalp.
What medical treatments are available for scalp eczema?
Options include topical corticosteroids, non‑steroidal calcineurin inhibitors, antifungal shampoos, oral antihistamines, and short courses of systemic steroids for severe cases.
What home care tips can help manage scalp eczema?
Use gentle sulfate‑free shampoos, avoid hot water, pat dry, limit alcohol‑based styling products, and apply moisturising scalp oils or ointments regularly.
How can I prevent scalp eczema from recurring?
Maintain scalp hydration, follow a balanced omega‑3 rich diet, manage stress, avoid known irritants, and schedule regular dermatologist follow‑ups.





