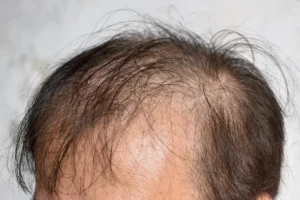
Many patients wonder does blood pressure medicine cause hair loss and how to differentiate normal shedding from medication‑induced alopecia. High blood pressure (hypertension) affects millions worldwide, and the drugs used to control it are essential for preventing heart attacks and strokes. However, a noticeable side effect for some users is thinning hair, which can be distressing and impact confidence.
Recent surveys indicate that up to 12 % of individuals on antihypertensive therapy report increased hair shedding within the first few months of treatment. While not all blood pressure drugs trigger this reaction, understanding the mechanisms and identifying the culprits can help you make informed decisions with your healthcare provider.
This article explores the relationship between blood pressure medication and hair loss, highlights the drugs most commonly implicated, offers practical steps to manage the side effect, and explains when professional evaluation is warranted. Armed with this knowledge, you can maintain both cardiovascular health and a healthy head of hair.
Understanding How Blood Pressure Medications Work
Blood pressure medicines, also known as antihypertensives, lower arterial pressure through several physiological pathways. The most common classes include:
- Angiotensin‑converting enzyme (ACE) inhibitors
- Angiotensin II receptor blockers (ARBs)
- Calcium channel blockers
- Beta‑blockers
- Diuretics
Each class targets a specific component of the renin‑angiotensin‑aldosterone system or vascular smooth muscle tone. While these mechanisms are vital for cardiovascular protection, they can also influence hair follicles indirectly by altering hormone levels, blood flow, or nutrient delivery to the scalp.
| Drug Class | Typical Examples | Vaak voorkomende bijwerkingen | Reported Hair‑Loss Incidence |
|---|---|---|---|
| ACE Inhibitors | Lisinopril, Enalapril | Cough, elevated potassium | Rare |
| ARBs | Losartan, Valsartan | Dizziness, hyperkalemia | Occasional |
| Calcium Channel Blockers | Amlodipine, Diltiazem | Swelling, flushing | Low‑to‑moderate |
| Beta‑Blockers | Metoprolol, Atenolol | Fatigue, cold extremities | Low |
| Diuretics | Hydrochlorothiazide, Furosemide | Frequent urination, electrolyte imbalance | Rare |
Understanding these pathways helps clinicians weigh the benefits of blood pressure control against potential dermatological side effects. The next section delves into the specific drugs most frequently linked to hair loss.

Which Blood Pressure Drugs Are Most Frequently Linked to Hair Loss?
Although the overall risk is low, certain antihypertensives have been documented in clinical reports and patient forums as more likely to cause alopecia. The following list highlights those agents:
- Amlodipine – Some studies suggest a modest association with telogen effluvium.
- Losartan – Case reports describe reversible hair thinning after several weeks.
- Metoprolol – Beta‑blockers can disrupt the hair growth cycle in susceptible individuals.
- Hydrochlorothiazide – Rarely linked to diffuse hair shedding.
Research on whether does blood pressure medicine cause hair loss remains mixed, but the pattern above aligns with the most frequently cited “blood pressure medication side effects” in patient surveys.
| Drug | Class | Evidence Level | Hair‑Loss Mechanism (Proposed) |
|---|---|---|---|
| Amlodipine | Calcium Channel Blocker | Moderate (case series) | Reduced scalp blood flow |
| Losartan | ARB | Low (isolated reports) | Hormonal modulation |
| Metoprolol | Beta‑Blocker | Low (case reports) | Interference with hair‑follicle cycling |
| Hydrochlorothiazide | Diuretic | Rare (single case) | Electrolyte imbalance affecting keratinisation |
If you are taking one of these medications and notice increased shedding, it does not automatically mean the drug must be stopped. A thorough evaluation can determine whether the hair loss is drug‑related or due to another factor such as stress, nutritional deficiency, or an underlying thyroid condition.
Identifying Hair Loss as a Medication Side Effect
Distinguishing drug‑induced hair loss from other causes requires a systematic approach. Key steps include:
- Document the timing of hair shedding relative to medication initiation.
- Review the medication list for known culprits (e.g., amlodipine, losartan).
- Assess for other symptoms such as scalp itching, scaling, or systemic signs.
- Consider a temporary medication pause under physician supervision to observe changes.
- Order basic labs (CBC, thyroid panel, iron studies) to rule out non‑drug factors.
Many patients ask, “does blood pressure medicine cause hair loss?” The answer hinges on the temporal relationship and exclusion of alternative diagnoses. In clinical practice, the phrase “blood pressure medication side effects” often encompasses fatigue, dizziness, and occasionally hair thinning, especially when the patient reports the onset shortly after starting therapy.
When the pattern suggests a medication link, clinicians may switch to an alternative with a lower reported incidence of alopecia. For example, moving from amlodipine to an ACE inhibitor like lisinopril, which has a rarer association with hair loss, can be an effective strategy.
Managing Hair Loss While Continuing Treatment
If discontinuing the antihypertensive is not advisable, several measures can mitigate hair loss without compromising blood pressure control:
- Topical minoxidil 5 % solution applied twice daily.
- Supplementation with biotin, zinc, and vitamin D after confirming deficiencies.
- Gentle hair‑care practices: avoid tight hairstyles, harsh chemicals, and excessive heat.
- Regular scalp massage to improve local circulation.
- Consider adding a low‑dose finasteride for male pattern involvement, under specialist guidance.
These interventions address the “blood pressure meds side effects” spectrum by targeting the hair‑loss component specifically. Additionally, discussing “blood pressure medicines with fewest side effects” with your physician can lead to a regimen that balances cardiovascular safety with dermatological comfort.
For patients experiencing significant thinning, referral to a dermatologist or a hair‑restoration specialist is advisable. Early treatment often yields better outcomes, and at Gold City Medical Center we integrate medical and cosmetic expertise to tailor a comprehensive plan.
When to Seek Professional Help for Hair Loss
Persistent or rapidly progressing hair loss warrants prompt medical attention. Indicators that you should schedule a consultation include:
- Shedding exceeding 100 hairs per day for more than two weeks.
- Visible bald patches or recession of the hairline.
- Associated scalp symptoms (pain, redness, scaling).
- Concurrent systemic signs such as unexplained weight loss or fatigue.
Specialists can differentiate alopecia caused by medication from autoimmune or hormonal conditions. In cases where the antihypertensive is essential, a dermatologist may recommend adjunctive therapies like platelet‑rich plasma (PRP) or low‑level laser therapy to stimulate follicular activity.
Gold City Medical Center offers an integrative approach: our physicians evaluate cardiovascular needs, while our cosmetic team provides personalized hair‑restoration solutions, including advanced hair transplant techniques when appropriate. This collaborative model ensures that patients receive comprehensive care without sacrificing either heart health or aesthetic goals.
Lifestyle Measures That Support Hair Health During Hypertension Therapy
Beyond medication management, everyday habits play a crucial role in maintaining a healthy scalp. Incorporate the following lifestyle strategies:
- Consume a balanced diet rich in lean proteins, omega‑3 fatty acids, and antioxidants.
- Stay hydrated to ensure optimal circulation to the scalp.
- Engage in regular aerobic exercise, which improves overall blood flow and reduces stress‑related hair shedding.
- Limit alcohol and tobacco use, both of which can exacerbate vascular constriction.
- Prioritize sleep; 7‑9 hours nightly supports hormonal balance and tissue repair.
These recommendations align with the broader goal of controlling high blood pressure while simultaneously fostering an environment conducive to hair growth. When combined with appropriate medical oversight, they can substantially reduce the likelihood that “blood pressure medication side effects” manifest as noticeable hair loss.
Why Choose Gold City Medical Center
Gold City Medical Center blends cutting‑edge medical expertise with aesthetic excellence. Our multidisciplinary team specializes in cardiovascular health, dermatology, and advanced hair‑restoration procedures, ensuring that patients receive coordinated care tailored to their unique needs. With a commitment to evidence‑based treatment and personalized attention, we help you manage hypertension without compromising your confidence.
Ready to protect your heart and your hair? Contact Gold City Medical Center today to schedule a comprehensive evaluation and discover personalized solutions for blood pressure management and hair health.
Call us or fill out our online consultation form – your journey to healthier circulation and fuller hair starts now.
FAQ
Can blood pressure medication cause hair loss?
Yes, some antihypertensive drugs have been reported to trigger hair shedding in a minority of patients.
Which antihypertensive drugs are most commonly associated with hair loss?
Amlodipine, losartan, metoprolol, and hydrochlorothiazide are the most frequently cited.
How can I tell if my hair loss is caused by my blood pressure medication?
Track timing, review drug lists, and rule out other causes with labs and clinical evaluation.
What can I do to manage hair loss without stopping my blood pressure medicine?
Use topical minoxidil, supplement deficiencies, adopt gentle hair‑care, and consider low‑dose finasteride if appropriate.
When should I see a dermatologist for medication‑related hair loss?
If shedding exceeds 100 hairs per day for two weeks, or you notice bald patches, pain, or systemic symptoms.