Fungal acne, often mistaken for ordinary acne, is a skin condition caused by an overgrowth of yeast that lives on the surface of the skin. While traditional acne is driven by bacteria, fungal acne stems from the Malassezia yeast, leading to a distinct set of symptoms that can be frustrating and persistent. This article explains the nature of fungal acne, outlines why it frequently appears on the forehead, chest, and back, and provides practical steps to clear it effectively.
Every year, millions of people worldwide experience breakouts that itch, especially after using heavy moisturizers or oily cosmetics. According to recent dermatological surveys, up to 30% of persistent acne cases may actually be fungal in origin. Recognizing the difference early can prevent months of unnecessary treatments and skin irritation.
In the sections that follow, we will explore the science behind Malassezia, identify common triggers, present proven treatment options—including antifungal creams for fungal acne—and share skincare habits that keep the yeast at bay. Whether you are dealing with occasional itchy pimples or a full‑body rash, understanding the root cause is the first step toward lasting relief.
What Is Fungal Acne and How It Differs From Bacterial Acne
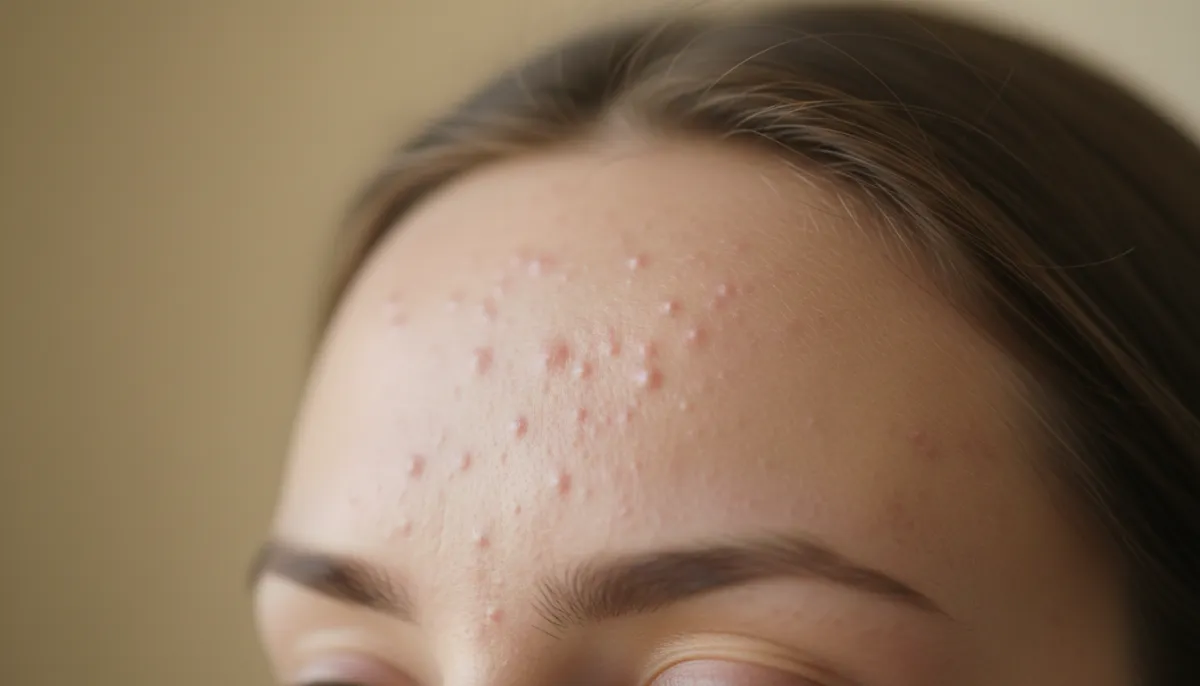
Fungal acne, medically referred to as Malassezia folliculitis or pityrosporum folliculitis, manifests as uniform, itchy pustules that often cluster on oily areas of the skin. Unlike bacterial acne, which typically produces deeper, inflamed nodules, fungal acne lesions are usually small, superficial, and may have a white or yellow head. The condition is caused by the yeast Malassezia, which thrives in warm, humid environments and feeds on skin lipids.
Key distinguishing features include:
- Uniform, monomorphic bumps that are often itchy rather than painful.
- Rapid spreading after using heavy, occlusive products.
- Limited response to traditional acne medications such as benzoyl peroxide.
A simple visual comparison helps clarify the differences:
| Feature | Bacterial Acne | Fungal Acne (Malassezia Folliculitis) |
|---|---|---|
| Typical Lesion | Papules, pustules, nodules | Uniform, itchy pustules |
| Common Locations | Forehead, nose, chin | Forehead, chest, back, shoulders |
| Response to Benzoyl Peroxide | Often effective | Usually ineffective |
| Trigger Factors | Hormonal changes, bacteria buildup | Excess oil, humidity, occlusive skincare |
Because the underlying cause is a yeast infection rather than bacterial proliferation, treatment strategies must target the fungus directly. Recognizing these signs early can save time and reduce the risk of chronic irritation.
Common Causes and Risk Factors for Malassezia Overgrowth
Understanding why Malassezia thrives is essential for preventing fungal acne. The yeast naturally resides on the skin, but certain conditions can tip the balance toward overgrowth. Key risk factors include:
- Excessive sebum production, often linked to hormonal fluctuations.
- Use of oily or comedogenic skincare products that create a barrier for the yeast.
- High humidity and sweating, especially in warm climates.
- Antibiotic use that disrupts the skin’s bacterial flora, allowing yeast to dominate.
- Compromised immune function, such as in individuals with diabetes or chronic stress.
Diet can also influence skin oiliness. Foods high in saturated fats and refined sugars may increase sebum output, indirectly promoting Malassezia proliferation. Additionally, certain fabrics—tight, synthetic materials—can trap heat and moisture, creating an ideal environment for fungal growth.
Below is a concise checklist for identifying potential triggers:
| Trigger | Typical Signs |
|---|---|
| Heavy moisturizers | Increased itchiness, new pustules |
| Frequent sweating | Breakouts after workouts |
| Antibiotic courses | Onset of acne‑like lesions weeks after treatment |
| High‑glycemic diet | Oilier skin, more frequent flare‑ups |
By systematically reviewing these factors, you can pinpoint the most likely contributors to your own fungal acne and begin to adjust habits accordingly.
Effective Treatments: From Topical Antifungals to Lifestyle Changes
When it comes to treating fungal acne, the most reliable approach combines medical therapy with lifestyle adjustments. The cornerstone of fungal acne treatment is the use of antifungal agents that specifically target Malassezia. Commonly prescribed options include topical creams such as ketoconazole, ciclopirox, and selenium sulfide, as well as oral antifungal medications like itraconazole or fluconazole for more severe cases.
Topical antifungal creams for fungal acne are typically applied twice daily for a period of two to four weeks. For stubborn lesions, a short course of oral antifungal medication may be recommended, especially when the infection has spread to larger body areas.
In addition to medication, the following supportive measures enhance outcomes:
- Switch to a non‑comedogenic cleanser that gently removes excess oil without stripping the skin.
- Incorporate a weekly exfoliating routine using salicylic acid to keep pores clear.
- Use a lightweight, oil‑free moisturizer to maintain barrier function without feeding the yeast.
- Wear breathable fabrics and change out of sweaty clothing promptly after exercise.
Below is a comparison of common treatment modalities:
| Behandeling | Application | Typical Duration | Pros | Cons |
|---|---|---|---|---|
| Ketoconazole 2% cream | Topical, twice daily | 2–4 weeks | Effective for mild to moderate cases | May cause mild irritation |
| Oral itraconazole | Systemic, once daily | 1–2 weeks | Rapid clearance of extensive lesions | Potential liver impact, requires monitoring |
| Salicylic acid cleanser | Topical, daily | Ongoing | Helps prevent pore blockage | Insufficient alone for fungal infection |
Patients often wonder whether over‑the‑counter products such as “Head & Shoulders” can help. While the active ingredient zinc pyrithione does have antifungal properties, it is generally less potent than prescription‑strength options. For best results, a dermatologist‑guided regimen is advisable.
Skincare Routine Adjustments to Prevent Recurrence
Even after successful treatment, maintaining a vigilant skincare routine is crucial to keep fungal acne at bay. The following step‑by‑step protocol can be incorporated into daily habits:
- Reinigen with a gentle, sulfate‑free cleanser that removes excess oil without disrupting the skin’s natural microbiome.
- Apply a lightweight, oil‑free moisturizer containing ingredients like hyaluronic acid or glycerin to support barrier repair.
- Use a targeted antifungal leave‑on product (e.g., a ketoconazole serum) a few times per week, especially in high‑risk zones.
- Exfoliate once or twice weekly with a salicylic acid pad to prevent follicular blockage.
- Finish with a broad‑spectrum sunscreen that is non‑comedogenic, protecting skin from UV‑induced inflammation.
Additional lifestyle tips include:
- Showering promptly after sweating to reduce moisture buildup.
- Avoiding heavy, oil‑based makeup during flare‑ups.
- Choosing breathable, cotton fabrics for sleepwear.
- Limiting intake of high‑glycemic foods that can increase sebum production.
By adhering to this routine, most individuals notice a significant reduction in the frequency of itchy pimples and can maintain clearer skin long term.
Why Choose Gold City Medical Center
Gold City Medical Center offers an integrative approach that combines dermatological expertise with personalized cosmetic care. Our team of board‑certified specialists evaluates each case of fungal acne individually, ensuring that treatment plans address both the underlying yeast overgrowth and any contributing lifestyle factors. With state‑of‑the‑art facilities, we provide prescription‑grade antifungal therapies, advanced skin analysis, and tailored skincare recommendations—all aimed at delivering lasting, healthy results. Trust our comprehensive care to restore confidence in your skin.
Ready to break free from itchy, persistent breakouts? Contact Gold City Medical Center today to schedule a personalized consultation and start your journey toward clear, comfortable skin.
Call us or fill out our online form—our specialists are waiting to help you.
FAQ
What is fungal acne and how is it different from regular acne?
Fungal acne, also called Malassezia folliculitis, is caused by yeast overgrowth and appears as uniform, itchy pustules, unlike bacterial acne which produces deeper, inflamed nodules.
What factors cause Malassezia overgrowth leading to fungal acne?
Excess sebum, humid environments, occlusive skincare, antibiotics, and a compromised immune system can all promote Malassezia overgrowth.
Which skincare products can trigger fungal acne?
Heavy, oily moisturizers, comedogenic creams, and products containing fatty acids can exacerbate fungal acne.
What are the most effective treatments for fungal acne?
Topical antifungal creams like ketoconazole, oral antifungals for severe cases, and supportive skin‑care measures are the cornerstone of treatment.
How can I prevent fungal acne from recurring?
Adopt a consistent, oil‑free skincare routine, avoid humid and occlusive environments, and monitor diet and lifestyle triggers.
Can over‑the‑counter shampoos like Head & Shoulders treat fungal acne?
They contain zinc pyrithione, which has mild antifungal activity, but are less potent than prescription‑strength treatments.
When should I see a dermatologist for fungal acne?
If breakouts persist after two weeks of over‑the‑counter care, become widespread, or cause significant discomfort, professional evaluation is advised.





