Dermatitis rash is a common skin condition that affects millions worldwide, often causing discomfort and visible irritation. This article explores the underlying causes, how to recognize the signs, and the most effective treatment pathways available today. According to recent dermatology surveys, up to 20% of adults experience some form of dermatitis during their lifetime, highlighting the importance of accurate information and timely care.
We will break down the different types of dermatitis, discuss what triggers flare‑ups, and provide practical guidance on managing symptoms at home and in clinical settings. Whether you suspect contact dermatitis, atopic dermatitis, or another form of eczema rash, understanding the disease process empowers you to take control of your skin health.
Our comprehensive overview is designed for anyone seeking clear, evidence‑based advice—from patients experiencing their first rash to those looking to prevent future episodes. By the end of this guide, you will know when to seek professional help, which treatments are most appropriate, and how to integrate skin‑care routines that support lasting relief.
Causes and Types of Dermatitis Rash
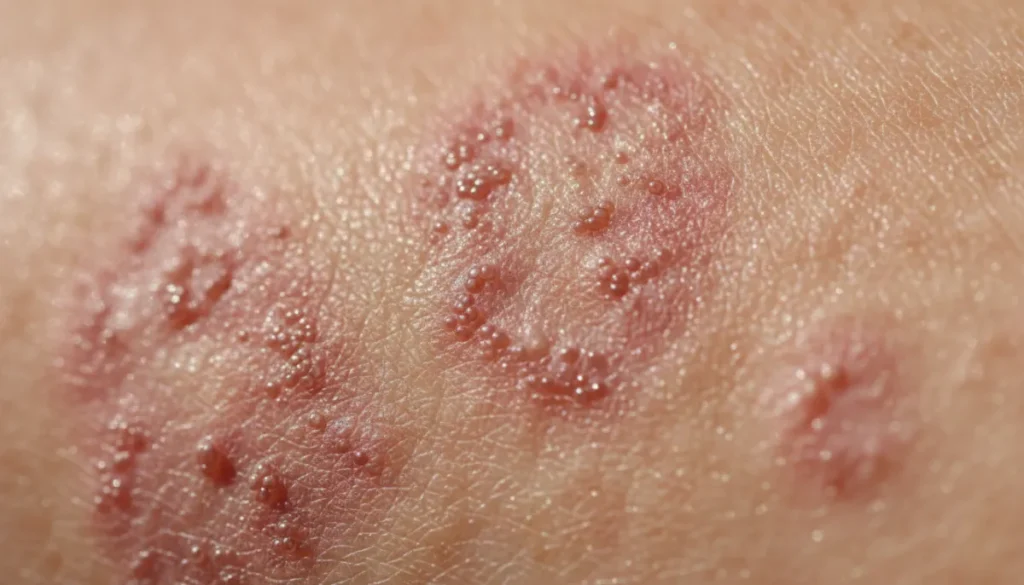
Dermatitis rash can arise from a variety of internal and external factors. The most frequently encountered forms include:
- Contact dermatitis: Triggered by direct skin contact with irritants or allergens such as chemicals, metals, or plants.
- Atopic dermatitis (often referred to as eczema): A chronic, genetically predisposed condition characterized by dry, itchy skin.
- Allergic dermatitis: Resulting from an immune response to substances like fragrances, preservatives, or certain fabrics.
- Irritant contact dermatitis: Caused by repeated exposure to harsh substances (e.g., detergents) that damage the skin barrier.
Understanding the distinction between these types is crucial because each may require a different therapeutic approach. For instance, allergic dermatitis typically responds well to avoidance strategies and antihistamines, whereas irritant contact dermatitis benefits from barrier repair creams and minimizing exposure.
| Type | Typical Trigger | Belangrijkste kenmerken |
|---|---|---|
| Contact Dermatitis | Allergens (nickel, poison ivy) | Red patches, itching, sometimes blisters |
| Atopic Dermatitis | Genetic predisposition, dry skin | Chronic itching, lichenified plaques |
| Allergic Dermatitis | Food, medications, cosmetics | Widespread rash, often with swelling |
| Irritant Contact Dermatitis | Soap, cleaning agents | Localized redness, burning sensation |
Other less common contributors include fungal infections, heat rash, and certain systemic diseases that manifest as skin eruptions. A thorough medical history and, when necessary, patch testing help clinicians pinpoint the exact cause, allowing for targeted treatment.
Recognizing Symptoms and When to Seek Care
Identifying a dermatitis rash early can prevent complications such as infection or chronic skin damage. Common symptoms include:
- Redness or discoloration of the skin.
- Itching, burning, or stinging sensations.
- Dry, scaly patches or flaky skin.
- Small blisters or vesicles that may ooze.
- Swelling and tenderness in the affected area.
While many rashes are benign, certain warning signs warrant prompt medical evaluation:
- Rapid spreading of the rash across large body areas.
- Severe pain, fever, or chills accompanying the skin changes.
- Signs of infection such as pus, crusting, or foul odor.
- Persistent rash lasting more than two weeks despite home care.
Patients with underlying conditions like asthma, hay fever, or a family history of atopy are more susceptible to severe atopic dermatitis. In such cases, early intervention by a dermatologist or an integrative health specialist can reduce the risk of chronic flare‑ups.
| Symptom | Typical Duration | When to Seek Help |
|---|---|---|
| Mild itching | Days to weeks | If it interferes with sleep or daily activities |
| Red patches | Up to 2 weeks | If spreading rapidly or becoming painful |
| Blisters or ooze | Variable | If signs of infection appear |
| Chronic dry skin | Months | If unresponsive to moisturizers |
At Gold City Medical Center, clinicians perform a detailed skin examination and may order additional tests—such as skin biopsies or allergy panels—to confirm the diagnosis and rule out other skin diseases.
Treatment Options: From Topical Care to Advanced Therapies
Treatment strategies for a dermatitis rash are tailored to the type, severity, and individual patient factors. The cornerstone of therapy is restoring the skin barrier and reducing inflammation.
Topical Therapies
First‑line options include:
- Corticosteroid creams (e.g., hydrocortisone 1% for mild cases, clobetasol for severe inflammation).
- Calcineurin inhibitors such as tacrolimus ointment, useful for sensitive areas like the face.
- Moisturizers enriched with ceramides, glycerin, and hyaluronic acid to reinforce barrier function.
These agents are typically applied two to three times daily, with the frequency adjusted based on response and side‑effect profile.
Systemic Medications
When topical measures are insufficient, doctors may prescribe oral medications:
- Antihistamines to alleviate itching.
- Systemic corticosteroids for short‑term control of severe flare‑ups.
- Immunomodulators such as cyclosporine or methotrexate for chronic atopic dermatitis.
Biologic agents (e.g., dupilumab) have emerged as highly effective for moderate‑to‑severe atopic dermatitis, offering targeted inhibition of specific inflammatory pathways.
Adjunctive and Natural Approaches
Integrative treatments can complement conventional therapy. Options include:
- Colloidal oatmeal baths to soothe itching.
- Cold compresses for immediate relief of heat‑induced rash.
- Topical applications of natural oils (e.g., coconut oil) with proven barrier‑repair properties.
Patients should discuss any complementary remedies with their provider to avoid interactions with prescribed medications.
| Therapie | Indication | Typical Duration |
|---|---|---|
| Topical steroids | Mild‑moderate dermatitis rash | 2–4 weeks, taper as needed |
| Calcineurin inhibitors | Sensitive‑area involvement | Ongoing, monitor for irritation |
| Systemic steroids | Severe acute flare‑up | Short course (≤2 weeks) |
| Biologics (dupilumab) | Moderate‑severe atopic dermatitis | Long‑term maintenance |
Gold City Medical Center’s multidisciplinary team evaluates each case individually, ensuring that the selected regimen aligns with the patient’s overall health, lifestyle, and cosmetic goals.
Managing Triggers and Preventing Recurrence
Prevention is a vital component of long‑term skin health. Identifying and minimizing exposure to known irritants can dramatically reduce the frequency of dermatitis rash episodes.
Environmental and Lifestyle Adjustments
Key strategies include:
- Wearing protective gloves when handling chemicals or cleaning agents.
- Choosing fragrance‑free, hypoallergenic skincare products.
- Maintaining optimal indoor humidity (40–60%) to prevent skin dryness.
- Using gentle, pH‑balanced soaps and avoiding hot water baths.
Allergy Identification
Patch testing remains the gold standard for pinpointing allergens responsible for contact dermatitis. Once identified, patients can eliminate the offending substances from their daily routine.
Skin Barrier Maintenance
Regular application of moisturizers—preferably within three minutes of bathing—helps lock in moisture and fortify the barrier against irritants. Ingredients such as ceramides, niacinamide, and panthenol are especially beneficial.
| Preventive Measure | Recommended Frequency | Key Benefit |
|---|---|---|
| Moisturizer application | 2–3 times daily | Reinforces barrier, reduces dryness |
| Humidifier use | Seasonal or year‑round | Prevents skin dehydration |
| Protective gloves | During exposure to irritants | Minimizes direct contact |
| Allergen avoidance | Continuous after identification | Reduces recurrence risk |
Adopting these habits not only curtails flare‑ups but also supports overall skin resilience, making future dermatitis rash episodes less severe and shorter in duration.
Lifestyle and Home Care Strategies for Healthy Skin
Beyond medical treatment, everyday choices greatly influence skin condition. A balanced diet rich in omega‑3 fatty acids, antioxidants, and vitamins can improve skin barrier function and reduce inflammation.
Nutrition Tips
- Include fatty fish (salmon, mackerel) or plant‑based sources (flaxseed, walnuts) for essential fatty acids.
- Consume colorful fruits and vegetables high in vitamin C and polyphenols.
- Stay hydrated; aim for at least 2 liters of water daily.
- Limit processed foods and excessive sugar, which may exacerbate inflammation.
Stress Management
Psychological stress is a known trigger for atopic dermatitis flare‑ups. Incorporating relaxation techniques such as mindfulness meditation, yoga, or gentle exercise can lower cortisol levels and improve skin outcomes.
Sleep Hygiene
Adequate sleep (7–9 hours per night) supports skin regeneration. Using breathable bedding and maintaining a cool bedroom temperature helps prevent night‑time itching that can worsen a rash.
By integrating these lifestyle adjustments with the clinical interventions described earlier, patients can achieve lasting relief from dermatitis rash and maintain healthier, more resilient skin.
Why Choose Gold City Medical Center
Gold City Medical Center combines cutting‑edge dermatological expertise with an integrative approach to health and beauty. Our multidisciplinary team offers personalized assessments, state‑of‑the‑art diagnostic tools, and treatment plans that blend conventional medicine with evidence‑based complementary therapies. Whether you need precise allergy testing, advanced biologic options, or holistic skin‑care guidance, we prioritize patient‑centered care that aligns with your lifestyle and aesthetic goals.
Ready to reclaim comfortable, clear skin? Contact Gold City Medical Center today to schedule a comprehensive skin assessment and discover a treatment plan tailored just for you.
Call us or visit our clinic to start your journey toward lasting relief from dermatitis rash.
FAQ
What are the common causes of dermatitis rash?
Dermatitis rash can be triggered by allergens, irritants, genetics, and environmental factors.
How can I differentiate between contact dermatitis and atopic dermatitis?
Contact dermatitis is usually localized to areas of exposure, while atopic dermatitis is chronic and often affects flexural sites.
When should I seek medical care for a skin rash?
Seek care if the rash spreads quickly, is painful, shows signs of infection, or lasts more than two weeks despite home treatment.
What are the first‑line topical treatments for dermatitis rash?
First‑line topical therapies include corticosteroid creams, calcineurin inhibitors, and moisturizers with barrier‑repair ingredients.
When are systemic medications or biologics needed for dermatitis?
Systemic treatments are considered for severe or refractory cases that do not respond to topical therapy.
How can I prevent future dermatitis flare‑ups?
Prevention focuses on identifying triggers, protecting the skin, and maintaining a healthy skin barrier.