If you are wondering how to stop hair loss from blood thinners, you are not alone. Many patients prescribed anticoagulant medication notice unexpected thinning or shedding of hair, which can be distressing and affect confidence. Understanding the link between these drugs and hair health is the first step toward effective management. In this article we explore why blood thinners can trigger hair loss, identify early warning signs, and present medical, lifestyle, and procedural solutions that empower you to regain control of your appearance while staying safe on essential medication.
Hair loss associated with medication is often overlooked because the primary focus is on the condition being treated—such as preventing blood clots. However, the impact on your scalp can be significant, especially if the loss is rapid or occurs in patches. By recognizing the underlying mechanisms, you can work with your healthcare team to adjust treatment plans, incorporate supportive therapies, and minimize the aesthetic side effects without compromising cardiovascular safety.
Throughout the following sections we will discuss the most common blood thinners, the biological pathways that lead to follicle disruption, practical steps you can take at home, and the advanced procedures available at Gold City Medical Center for those seeking lasting restoration.
Understanding Why Blood Thinners Trigger Hair Loss
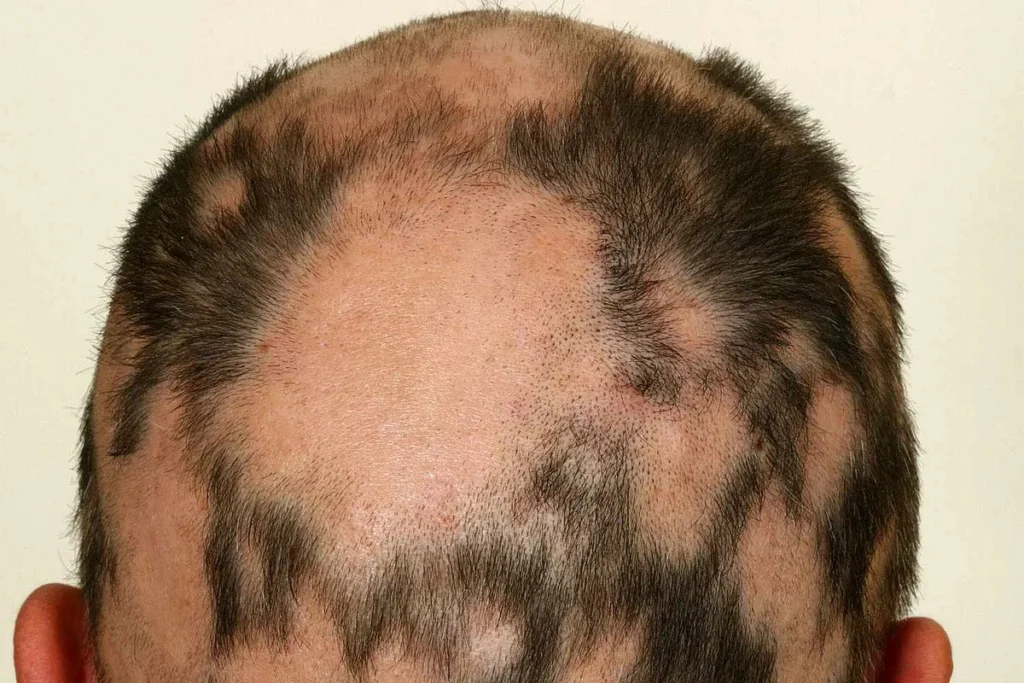
Blood thinners, also known as anticoagulants, work by interfering with the clotting cascade to reduce the risk of thrombosis. While life‑saving, these drugs can unintentionally affect the hair growth cycle. The most common mechanism involves reduced blood flow to the scalp, which limits the delivery of oxygen and essential nutrients to hair follicles. Additionally, some anticoagulants alter hormonal balances or trigger an inflammatory response that accelerates the telogen (resting) phase, leading to diffuse shedding.
Common blood thinners linked to hair loss include:
- Warfarin (Coumadin)
- Apixaban (Eliquis)
- Rivaroxaban (Xarelto)
- Dabigatran (Pradaxa)
- Heparin (unfractionated and low‑molecular‑weight)
Research on medications that cause hair loss indicates that the incidence varies by individual genetics, dosage, and duration of therapy. For example, patients on long‑term warfarin may experience a higher rate of diffuse alopecia compared with those using newer direct oral anticoagulants (DOACs). Understanding which specific medication you are taking helps your physician assess risk and consider alternatives if appropriate.
It is also worth noting that other prescription drugs, such as certain antihypertensives (e.g., amlodipine) or cholesterol‑lowering agents (e.g., atorvastatin), can compound the problem when used alongside blood thinners. A comprehensive medication review is essential to isolate the primary culprit.
Identifying Early Signs and When to Seek Help
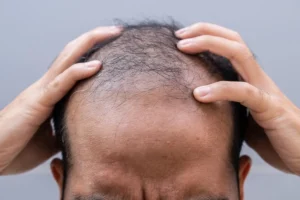
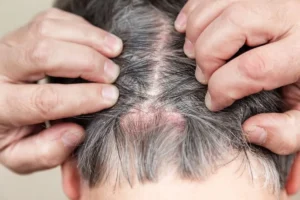
Recognizing hair loss early can prevent extensive thinning and improve treatment outcomes. The most common early signs include:
- Increased shedding during washing or brushing
- Noticeable thinning on the crown or frontal scalp
- Small, round bald patches that develop over weeks
- Overall reduction in hair density without an obvious external cause
If you observe any of these symptoms within the first three months of starting a blood thinner, schedule a consultation with your prescribing physician. While occasional shedding is normal, persistent or rapid loss may indicate that the medication is affecting the hair growth cycle.
During the visit, the clinician will typically perform a brief scalp examination and may request a blood test to rule out nutritional deficiencies (iron, zinc, vitamin D) that can mimic drug‑induced alopecia. Differentiating between telogen effluvium caused by medication and other forms of alopecia, such as androgenetic or autoimmune, ensures that the subsequent management plan is appropriately targeted.
Medical Strategies to Reduce Hair Loss While on Anticoagulants
When medication is essential for preventing serious clotting events, discontinuation is rarely an option. Instead, clinicians focus on mitigating side effects through dosage adjustment, supplemental therapy, and targeted topical agents. Below is a comparison of common medical approaches.
| Approach | How It Works | Typical Use Cases |
|---|---|---|
| Dosage Optimization | Lowering the dose while maintaining therapeutic INR or anti‑Xa levels | Patients with mild clotting risk or stable INR |
| Switch to Alternative Anticoagulant | Replacing warfarin with a DOAC that has a lower reported incidence of alopecia | Patients experiencing severe hair loss or intolerable side effects |
| Topical Minoxidil (5%) | Stimulates follicular blood flow and prolongs the anagen phase | Early‑stage diffuse shedding, used under dermatologist supervision |
| Oral Biotin or Zinc Supplementation | Supports keratin production and follicle health | Patients with documented deficiencies or low dietary intake |
| Low‑Level Laser Therapy (LLLT) | Photobiomodulation improves cellular metabolism in hair follicles | Adjunct for moderate thinning when topical agents are insufficient |
In addition to these options, some clinicians prescribe short courses of corticosteroids (e.g., prednisone) to reduce inflammation that may be exacerbating hair loss. However, systemic steroids carry their own risk profile and are used only when benefits clearly outweigh potential harms.
It is crucial to coordinate any changes with both your cardiologist and a dermatologist experienced in medication‑induced alopecia. This collaborative approach ensures that clotting protection remains optimal while hair health is actively supported.
Lifestyle and Nutritional Support for Hair Regrowth
While medical interventions address the direct effects of anticoagulants, lifestyle modifications can create an environment that encourages hair regrowth. A balanced diet rich in protein, essential fatty acids, and micronutrients supports the keratin structure of hair strands and sustains follicle activity.
Key nutrients to prioritize include:
- Eiwit: Lean meats, legumes, and dairy provide the building blocks for hair fibers.
- Omega‑3 fatty acids: Fatty fish (salmon, mackerel), chia seeds, and walnuts reduce inflammation and improve scalp circulation.
- Iron and zinc: Red meat, spinach, pumpkin seeds, and fortified cereals prevent deficiency‑related shedding.
- Biotin (vitamin B7): Eggs, almonds, and sweet potatoes promote healthy keratin synthesis.
- Vitamin D: Sun exposure and fortified dairy help regulate the hair growth cycle.
In addition to nutrition, stress management plays a pivotal role. Chronic stress elevates cortisol levels, which can push hair follicles into the telogen phase. Incorporating mindfulness practices, regular moderate exercise, and adequate sleep (7‑9 hours) can mitigate this effect.
Hydration is another often‑overlooked factor. Dehydrated scalp tissue becomes less resilient, making hair more prone to breakage. Aim for at least eight glasses of water daily, and consider herbal teas (e.g., green tea) that contain antioxidants beneficial for skin and hair health.
Procedural Options: From PRP to Hair Transplant
When conservative measures are insufficient, procedural interventions can provide noticeable and lasting results. Gold City Medical Center offers a suite of evidence‑based treatments tailored to the individual’s pattern of loss and overall health.
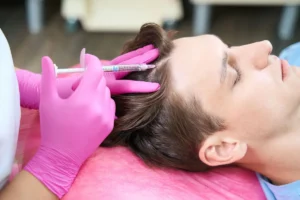
Platelet‑Rich Plasma (PRP) Therapy involves drawing a small amount of the patient’s blood, concentrating platelets, and injecting the plasma into the scalp. Growth factors released from the platelets stimulate dormant follicles and improve vascularization. PRP is especially effective for patients with early‑stage thinning and can be combined with topical minoxidil for synergistic benefit.
Microneedling creates micro‑injuries that trigger a wound‑healing response, encouraging new hair growth. When performed in conjunction with topical agents, microneedling enhances product absorption and follicular activation.
Follicular Unit Extraction (FUE) Hair Transplant is a surgical option for those with advanced or stable alopecia. Individual hair follicles are harvested from a donor area (typically the back of the scalp) and implanted into thinning zones. The procedure preserves natural hair direction and density, offering a permanent solution when donor supply is adequate.
Each of these options is evaluated based on the patient’s medical history, including the specific blood thinner regimen, to ensure safety and optimal outcomes. Our multidisciplinary team coordinates with cardiology to schedule procedures at times when anticoagulation levels are stable, minimizing bleeding risk.
Creating a Personalized Care Plan with Your Healthcare Team
Successful management of medication‑induced hair loss hinges on clear communication among all providers involved in your care. A typical care pathway includes:
- Initial assessment by your prescribing physician to confirm the link between the anticoagulant and hair loss.
- Referral to a dermatologist or hair restoration specialist for detailed scalp evaluation.
- Joint review of medication options, including potential dose reduction or switching to an alternative anticoagulant with a lower alopecia risk.
- Implementation of supportive therapies—nutritional supplements, topical agents, or procedural interventions—as recommended.
- Regular follow‑up appointments to monitor clotting parameters, hair regrowth progress, and any side effects.
This coordinated approach ensures that you do not compromise cardiovascular protection while actively addressing the aesthetic concerns that affect quality of life. By involving a specialist team early, adjustments can be made before hair loss becomes severe, often preserving the natural hair you already have.
Why Choose Gold City Medical Center
Gold City Medical Center combines integrative medicine with cutting‑edge hair restoration technology. Our multidisciplinary team—comprising cardiologists, dermatologists, and certified hair transplant surgeons—delivers personalized treatment plans that respect both your medical needs and cosmetic goals. With a focus on safety, evidence‑based practices, and patient‑centered care, we help you achieve lasting hair health without compromising the effectiveness of essential blood‑thinning therapy.
Ready to take control of your hair health? Contact Gold City Medical Center today to schedule a comprehensive evaluation and explore tailored solutions that work with your anticoagulant regimen.
Call us or fill out our online request form—your journey to fuller, healthier hair starts now.
FAQ
Why can blood thinners cause hair loss?
Blood thinners may reduce scalp blood flow, alter hormonal balance, or trigger inflammation, pushing hair follicles into the resting (telogen) phase.
What are the early signs of medication‑induced hair loss?
Early signs include increased shedding during washing, thinning on the crown or frontal scalp, small round bald patches, and overall reduced hair density.
Can I continue my blood thinner while treating hair loss?
Yes, discontinuation is rarely advisable; instead, doctors adjust dosage, switch agents, or add supportive therapies like minoxidil, supplements, or laser treatment.
What lifestyle changes support hair regrowth while on anticoagulants?
A balanced diet rich in protein, omega‑3s, iron, zinc, biotin, and vitamin D, along with stress management, adequate sleep, and proper hydration, can promote regrowth.
How effective is PRP therapy for blood‑thinner‑related hair loss?
PRP can stimulate dormant follicles and improve scalp vascularization, especially in early‑stage thinning, often enhancing results when combined with minoxidil.
When is a hair transplant considered for patients on blood thinners?
A transplant is considered when hair loss is stable, advanced, and the patient’s anticoagulation regimen can be safely managed during surgery.