Many people wonder what is dermatitis and why it appears as red, itchy patches on the skin. Dermatitis is a broad term that describes inflammation of the skin, which can result from a variety of internal and external factors. In this article we explain the condition, outline the most common types, and provide practical advice on managing symptoms.
Skin inflammation affects millions worldwide, with contact dermatitis alone accounting for a significant share of dermatology visits each year. Recognising the early signs—such as itching, swelling, and rash—can prevent complications and improve quality of life.
We will explore the underlying mechanisms, discuss how healthcare professionals diagnose dermatitis, and review treatment options ranging from topical creams to lifestyle adjustments. Whether you experience occasional flare‑ups or chronic irritation, understanding the condition is the first step toward effective care.
What Is Dermatitis? Definition and Common Signs
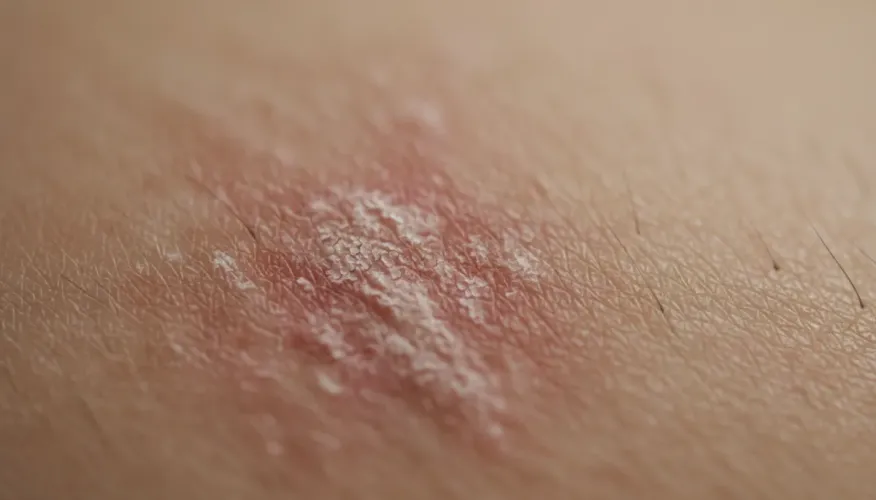
Dermatitis refers to inflammation of the skin that manifests as redness, swelling, and often itching. The condition can be acute, appearing suddenly and lasting a few days, or chronic, persisting for months or even years. Common signs include:
- Red or pink patches
- Itching or burning sensation
- Dry, scaly, or cracked skin
- Blisters or oozing lesions in severe cases
These symptoms may vary depending on the specific type of dermatitis and the individual’s skin sensitivity. While the term “rash” is frequently used interchangeably, not all rashes are dermatitis; some may be infections or allergic reactions unrelated to skin inflammation.
Identifying the pattern and location of the rash helps clinicians differentiate dermatitis from other skin conditions. For example, a rash that appears on the hands after handling cleaning products often points to contact dermatitis, whereas widespread itching on the elbows and knees may suggest atopic dermatitis.
Types of Dermatitis: From Atopic to Contact
Dermatitis encompasses several distinct forms, each with unique triggers and characteristics. Understanding these types helps patients and clinicians choose the most appropriate treatment.
Atopic Dermatitis (Eczema)
Atopic dermatitis is a chronic, relapsing condition often associated with a personal or family history of allergies, asthma, or hay fever. It typically begins in childhood and may affect the face, neck, and flexural areas such as elbows and knees.
Contact Dermatitis
Contact dermatitis occurs when the skin reacts to an external substance. It is divided into:
- Allergic contact dermatitis: An immune‑mediated response to allergens like nickel, fragrances, or latex.
- Irritant contact dermatitis: Direct damage from chemicals, detergents, or prolonged moisture.
Seborrheic Dermatitis
This type primarily affects oily areas of the body, such as the scalp, eyebrows, and nasolabial folds. It presents as greasy, yellowish scales and is linked to the yeast Malassezia.
Stasis Dermatitis
Stasis dermatitis develops in the lower legs of individuals with chronic venous insufficiency. Poor blood flow leads to fluid buildup, causing itching, redness, and sometimes ulceration.
| Type | Typical Location | Common Triggers | Key Features |
|---|---|---|---|
| Atopic Dermatitis | Face, neck, flexures | Genetic predisposition, allergens | Chronic, itchy, dry patches |
| Contact Dermatitis | Hands, wrists, exposed skin | Nickel, cosmetics, detergents | Redness, blisters, localized |
| Seborrheic Dermatitis | Scalp, eyebrows, chest | Yeast overgrowth, oily skin | Greasy scales, redness |
| Stasis Dermatitis | Lower legs | Venous insufficiency | Swelling, itching, brownish discoloration |
Causes and Triggers: Allergens, Irritants, and Genetics
Dermatitis arises from a combination of internal predispositions and external exposures. While genetics play a role—especially in atopic dermatitis—environmental factors often precipitate flare‑ups.
Allergic Triggers
Allergic contact dermatitis is triggered by substances that provoke an immune response. Common allergens include:
- Nickel in jewelry
- Fragrances in cosmetics
- Preservatives such as parabens
- Latex in gloves
Irritant Factors
Irritant contact dermatitis results from direct damage to the skin barrier. Frequent culprits are:
- Harsh detergents and soaps
- Solvents and cleaning agents
- Prolonged exposure to water
- Physical friction from clothing
Genetic and Immune Influences
Individuals with a family history of eczema or asthma are more likely to develop atopic dermatitis. Mutations in the filaggrin gene, which helps maintain skin barrier integrity, increase susceptibility to dryness and irritation.
Understanding personal triggers—whether they are allergens, irritants, or lifestyle factors—enables targeted prevention strategies, reducing the frequency and severity of flare‑ups.
Diagnosis and When to Seek Medical Help
Accurate diagnosis of dermatitis involves a thorough clinical evaluation. While many cases can be identified by visual inspection and patient history, certain situations require additional testing.
Clinical Examination
Dermatologists assess the distribution, appearance, and duration of the rash. They ask detailed questions about recent exposures, personal or family history of allergies, and lifestyle habits.
Patch Testing
For suspected allergic contact dermatitis, patch testing is the gold standard. Small amounts of potential allergens are applied to the skin under occlusive patches and observed over 48–72 hours for reactions.
When to Consult a Professional
Seek medical attention if you experience:
- Rapid spreading of the rash
- Severe pain, swelling, or fever
- Blisters that ooze or become infected
- Persistent symptoms despite over‑the‑counter treatment
Early intervention can prevent complications such as secondary infections or chronic skin changes, and it allows for personalized treatment planning.
Treatment Options: Skincare, Medications, and Lifestyle
Managing dermatitis requires a multifaceted approach that addresses inflammation, restores the skin barrier, and eliminates triggers.
Topical Therapies
First‑line treatments include:
- Corticosteroid creams to reduce inflammation
- Calcineurin inhibitors (e.g., tacrolimus) for sensitive areas
- Moisturizers and emollients to repair barrier function
Systemic Medications
For severe or widespread cases, doctors may prescribe oral antihistamines, systemic corticosteroids, or newer biologic agents that target specific immune pathways.
Lifestyle and Home Care
Effective self‑care strategies include:
- Identifying and avoiding known allergens or irritants.
- Using fragrance‑free, hypoallergenic skin products.
- Keeping skin moisturised after bathing with thick creams.
- Wearing breathable fabrics and avoiding excessive heat.
Combining medical treatment with preventive skin care maximises relief and reduces the likelihood of future flare‑ups.
Why Choose Gold City Medical Center
Gold City Medical Center offers integrative healthcare with a focus on personalized dermatological care. Our experienced physicians combine evidence‑based medicine with advanced treatment options to address the root causes of dermatitis. Whether you need a precise diagnosis, targeted topical therapy, or comprehensive lifestyle guidance, our team is dedicated to restoring your skin’s health and comfort. Trust a centre that blends medical expertise with a commitment to patient‑centered service.
Ready to take control of your skin health? Contact Gold City Medical Center today to schedule a consultation with our dermatology specialists. Experience tailored treatment plans that bring lasting relief and confidence.
FAQ
What causes dermatitis?
Dermatitis can be triggered by genetic factors, allergens, irritants, and environmental conditions.
What are the main types of dermatitis?
The main types include atopic dermatitis, contact dermatitis, seborrheic dermatitis, and stasis dermatitis.
How is dermatitis diagnosed?
Diagnosis is based on clinical examination, patient history, and sometimes patch testing.
When should I see a doctor for dermatitis?
Seek medical help if the rash spreads quickly, is painful, oozes, or doesn’t improve with over‑the‑counter care.
What treatment options are available for dermatitis?
Treatments include topical steroids, calcineurin inhibitors, moisturizers, oral antihistamines, systemic meds, and lifestyle changes.
Can lifestyle changes help manage dermatitis?
Yes, avoiding triggers, using gentle skin products, and keeping the skin moisturized can greatly improve symptoms.