Contact dermatitis is a common skin condition that arises when the skin reacts to an irritant or allergen. It affects millions worldwide, with an estimated 246,000 monthly searches indicating the level of public concern. In this article, we explore what contact dermatitis is, why it develops, and how you can manage it effectively. Whether you are dealing with a mild rash or a more persistent reaction, understanding the underlying mechanisms can help you make informed decisions about care.
We will cover the different types of dermatitis, the most frequent triggers, how to recognize symptoms, and the range of treatment options—from over‑the‑counter ointments to prescription‑strength topical steroids. You will also learn practical prevention strategies that can reduce the likelihood of future flare‑ups. By the end of this guide, you will have a clear roadmap for navigating this skin irritation and restoring comfort to your daily life.
Skin reactions can be frustrating, especially when they appear on visible areas such as the face or hands. The good news is that with the right approach, most cases of contact dermatitis can be controlled, allowing you to return to your regular activities without lingering discomfort.
What Is Contact Dermatitis and How It Develops
Contact dermatitis is an inflammatory skin response that occurs after direct contact with a substance that either irritates the skin or triggers an allergic reaction. The condition is broadly divided into two categories: allergic contact dermatitis and irritant contact dermatitis. Allergic contact dermatitis involves an immune‑mediated response, typically requiring prior sensitization to the allergen. In contrast, irritant contact dermatitis results from direct damage to the skin’s protective barrier, often after brief exposure to a harsh chemical.
The skin’s outer layer, the stratum corneum, acts as a barrier against external agents. When this barrier is compromised—by frequent hand washing, exposure to solvents, or prolonged wear of protective gloves—irritants can penetrate more easily, leading to inflammation. In allergic cases, the immune system mistakenly identifies a harmless substance (such as nickel, fragrance, or certain preservatives) as a threat, releasing histamine and other mediators that cause redness, itching, and swelling.
Understanding the underlying mechanism is crucial because it guides treatment choices. For example, allergic reactions often require avoidance of the specific allergen and may benefit from antihistamines, whereas irritant reactions may respond well to barrier repair creams and moisturizers.
Common Triggers and Risk Factors
Identifying the substances that provoke a reaction is the first step toward preventing future outbreaks. Below is a list of frequent triggers for both allergic and irritant forms of contact dermatitis:
- Nickel in jewelry and belt buckles
- Fragrances in cosmetics and detergents
- Preservatives such as parabens and formaldehyde releasers
- Rubber accelerators found in gloves and shoes
- Household cleaning agents, especially bleach and ammonia
- Plant oils (e.g., poison ivy, oak, and sumac)
- Metalworking fluids and solvents
Risk factors that increase susceptibility include a personal or family history of atopic dermatitis, frequent exposure to wet environments, and a compromised skin barrier due to chronic dryness. Individuals with a history of asthma or allergic rhinitis are also more likely to develop allergic contact dermatitis.
Understanding these triggers enables targeted avoidance strategies, which are often the most effective long‑term solution. For instance, substituting fragrance‑free products or using protective barriers when handling chemicals can significantly reduce the incidence of flare‑ups.
Recognizing Symptoms and When to Seek Care
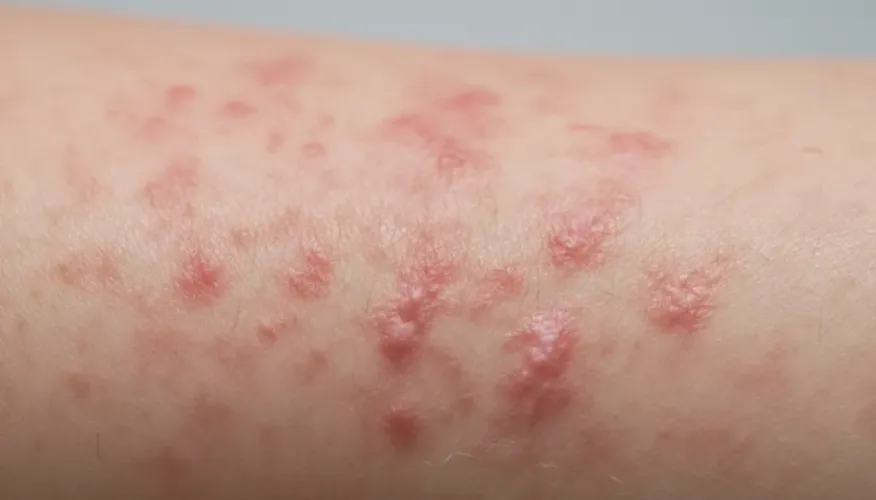
Symptoms of contact dermatitis typically appear within minutes to several days after exposure, depending on the type of reaction. Common signs include:
- Redness and swelling of the affected area
- Itching or burning sensation
- Blister formation or oozing lesions
- Dry, scaly patches once the rash begins to heal
- Swelling of the surrounding tissue (especially in severe cases)
While many cases are mild and resolve with self‑care, certain scenarios warrant professional evaluation:
- Rash spreading beyond the initial contact site
- Severe pain, fever, or swelling of lymph nodes
- Persistent symptoms lasting more than two weeks despite home treatment
- Involvement of sensitive areas such as the face, eyelids, or genitals
- Signs of infection, such as pus or increasing warmth
Prompt medical attention ensures accurate diagnosis—distinguishing contact dermatitis from other skin conditions like eczema or psoriasis—and facilitates appropriate therapy. Early intervention can also prevent complications such as secondary bacterial infection.
Treatment Options: From Topical Steroids to Advanced Therapies
Treatment strategies are tailored to the severity of the reaction and whether the underlying cause is allergic or irritant. Below is a comparison of common therapeutic approaches:
| Treatment | Indication | Typical Duration | Key Benefits |
|---|---|---|---|
| Topical corticosteroids | Moderate to severe inflammation | 1–2 weeks (short‑term) | Rapid reduction of redness and itching |
| Calcineurin inhibitors (e.g., tacrolimus) | Sensitive areas (face, eyelids) | 2–4 weeks | Steroid‑sparing, low irritation risk |
| Moisturizers & barrier creams | Mild irritation, prevention | Ongoing | Restores skin barrier, reduces recurrence |
| Antihistamines (oral) | Allergic itching | As needed | Relieves itch, improves sleep |
| Systemic steroids | Severe, widespread reactions | Short course | Controls extensive inflammation quickly |
For allergic contact dermatitis, avoidance of the identified allergen is essential. Patch testing, a diagnostic tool performed by a dermatologist, can pinpoint specific triggers, allowing for precise avoidance measures. In cases of irritant contact dermatitis, protective gloves, frequent moisturization, and gentle cleansing agents are the cornerstone of management.
When over‑the‑counter ointments fail to provide relief, prescription‑strength topical steroids or calcineurin inhibitors may be recommended. These medications should be used under medical supervision to minimize potential side effects such as skin thinning or steroid‑induced acne.
Prevention Strategies and Lifestyle Adjustments
Preventing future episodes of contact dermatitis hinges on a combination of environmental control, skin care routines, and awareness of personal sensitivities. Below are practical steps you can incorporate into daily life:
- Use fragrance‑free, hypoallergenic soaps and moisturizers.
- Wear protective gloves when handling chemicals, and choose cotton liners to reduce sweat buildup.
- Conduct a patch test before using new cosmetics or household products.
- Maintain a regular moisturizing regimen to keep the skin barrier intact.
- Limit exposure to known allergens, such as nickel jewelry, by opting for stainless‑steel or plastic alternatives.
- Keep nails short and clean to avoid trapping irritants under the nail plate.
For individuals who experience dermatitis on the face or nails, specific care is required. Gentle, non‑scratching cleansing, combined with non‑comedogenic moisturizers, can prevent irritation of delicate facial skin. Nail care should include the use of soft gloves and avoidance of harsh nail polishes containing formaldehyde.
Regular follow‑up with a dermatologist at Gold City Medical Center ensures that any emerging triggers are identified early, and treatment plans are adjusted accordingly. Consistency in preventive measures dramatically reduces the frequency of flare‑ups and improves overall skin health.
Why Choose Gold City Medical Center
Gold City Medical Center combines integrative medicine with cutting‑edge dermatology to provide comprehensive care for contact dermatitis. Our team of experienced specialists offers personalized assessment, advanced diagnostic testing, and a full spectrum of treatment options—from topical steroids to innovative barrier‑repair therapies. By integrating medical expertise with a focus on overall wellbeing, we ensure that each patient receives a tailored plan that addresses both the skin condition and underlying lifestyle factors.
Located in the heart of the city, our state‑of‑the‑art facility is equipped with modern diagnostic tools and comfortable treatment rooms. We prioritize patient education, empowering you to manage your skin health confidently and sustainably.
Ready to regain comfort and confidence? Contact Gold City Medical Center today to schedule a personalized dermatology consultation. Our experts will help you identify triggers, develop an effective treatment plan, and guide you toward lasting relief.
FAQ
What causes contact dermatitis?
Contact dermatitis is caused by exposure to irritants or allergens that damage the skin or trigger an immune response.
How can I tell if my rash is allergic or irritant contact dermatitis?
Allergic dermatitis usually requires prior sensitization and may involve widespread itching, while irritant dermatitis often appears after a single exposure and affects the area of contact.
What are the most common triggers for contact dermatitis?
Common triggers include nickel, fragrances, preservatives, rubber accelerators, cleaning agents, and plant oils like poison ivy.
When should I seek medical care for contact dermatitis?
Seek care if the rash spreads, causes severe pain, fever, lasts more than two weeks, or shows signs of infection.
What treatment options are available for contact dermatitis?
Treatments range from moisturizers and barrier creams to prescription topical steroids, calcineurin inhibitors, antihistamines, and systemic steroids for severe cases.
How can I prevent future flare‑ups of contact dermatitis?
Prevention includes using fragrance‑free products, wearing protective gloves, regular moisturization, and patch testing new items.