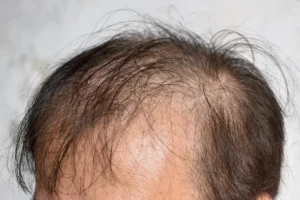
Experiencing scalp pain and hair loss can be unsettling, especially when the cause is unclear. This article explains the underlying mechanisms, common triggers, and practical steps you can take to restore comfort and healthy hair growth. According to recent dermatology surveys, up to 30% of adults notice some degree of scalp discomfort during their lifetime, and many associate it with increased shedding.
We will explore medical conditions such as alopecia, hormonal imbalances, and lifestyle factors that contribute to both pain and thinning strands. By understanding the link between the nervous system, skin health, and follicle activity, you can make informed decisions about when to seek professional help and which treatments may be most effective.
Whether you are dealing with a sudden patch of hair loss, persistent itching, or a burning sensation on the scalp, the information below will guide you through diagnosis, prevention, and therapeutic options tailored to individual needs.
Common Causes of Scalp Discomfort and Hair Shedding
Several medical and environmental factors can simultaneously trigger scalp pain and hair loss. Recognizing these causes is the first step toward targeted treatment.
- Inflammatory skin disorders such as seborrheic dermatitis and psoriasis often cause itching, redness, and flaking, which can irritate hair follicles.
- Traction alopecia results from tight hairstyles that pull on the scalp, leading to tension‑induced pain and gradual thinning.
- Infections including fungal (tinea capitis) and bacterial infections can produce painful lesions and accelerate shedding.
- Medication side effects – certain drugs (e.g., anticoagulants, retinoids) list scalp discomfort as a possible adverse reaction.
- Physical trauma – injuries, burns, or aggressive brushing can damage the scalp’s nerve endings and disrupt the growth cycle.
Below is a quick reference table summarizing the typical symptoms, primary triggers, and recommended initial actions.
| Condition | Key Symptoms | Typical Triggers | First‑Line Management |
|---|---|---|---|
| Seborrheic Dermatitis | Itchy, flaky scalp; mild pain | Excess oil, yeast overgrowth | Anti‑fungal shampoo, moisturising scalp treatment |
| Traction Alopecia | Tenderness along hairline; gradual thinning | Tight braids, ponytails | Loosen hairstyles, gentle scalp massage |
| Fungal Infection | Red patches, pustules, burning | Warm, humid environment | Topical antifungal medication |
| Medication‑Induced | Diffuse scalp soreness, diffuse shedding | Specific prescription drugs | Consult prescribing physician for alternatives |

How Dermatological Conditions Influence Hair Growth
Skin disorders that affect the scalp can directly interfere with the hair growth cycle. For instance, alopecia areata is an autoimmune condition where the body’s immune system attacks hair follicles, often causing smooth, round patches of hair loss accompanied by tingling or mild pain.
Another frequent culprit is seborrheic dermatitis scalp inflammation, which can create a hostile environment for follicles by increasing sebum production and fostering yeast proliferation. This irritation may lead to a temporary shift into the telogen phase, known as telogen effluvium, where a larger proportion of hairs enter the resting stage and fall out within weeks.
- Alopecia areata – sudden patchy loss, possible scalp soreness.
- Psoriasis – thick, silvery scales, burning sensation.
- Contact dermatitis – reaction to hair products, localized pain.
Effective management typically combines anti‑inflammatory therapy with supportive hair‑care practices. Topical corticosteroids, calcineurin inhibitors, or newer Janus kinase (JAK) inhibitors can reduce immune‑mediated attack, while gentle cleansing helps restore barrier function.
The Role of Hormones and Genetics in Hair Loss
Hormonal fluctuations and genetic predisposition are major drivers of androgenetic alopecia, commonly known as male or female pattern baldness. Dihydrotestosterone (DHT), a derivative of testosterone, binds to receptors in susceptible follicles, shortening the anagen (growth) phase and causing miniaturisation. While this process usually presents as a receding hairline or thinning crown, some individuals report accompanying scalp tenderness due to increased vascular sensitivity.
In women, estrogen decline during menopause can also shift follicles toward a shorter growth cycle, leading to diffuse thinning rather than distinct bald spots. Additionally, thyroid disorders—both hyper‑ and hypothyroidism—may cause scalp discomfort and increased shedding.
Genetic testing can identify variations in the AR gene that heighten DHT sensitivity. However, lifestyle factors such as stress, poor nutrition, and smoking can amplify genetic risk, making a comprehensive approach essential.
| Factor | Impact on Hair Follicles | Typical Symptoms |
|---|---|---|
| DHT (androgenic) | Follicle miniaturisation | Receding hairline, crown thinning |
| Estrogen decline | Shortened anagen phase | Diffuse thinning, occasional scalp tightness |
| Thyroid imbalance | Disrupted hair cycle | Hair shedding, dry scalp, occasional itching |
Targeted therapies such as oral finasteride, topical minoxidil, or low‑level laser therapy can counteract hormonal effects, while nutraceuticals support follicle health.
When to Seek Professional Evaluation and Treatment Options
If scalp pain persists for more than two weeks, is accompanied by swelling, pus, or sudden, extensive hair loss, it is advisable to consult a specialist. Early assessment allows clinicians to differentiate between benign conditions and those requiring medical intervention.
Diagnostic steps often include:
- Detailed medical history and scalp symptom questionnaire.
- Physical examination with dermatoscope to assess follicle health.
- Laboratory tests (thyroid panel, hormone levels, iron studies) to rule out systemic causes.
- Scalp biopsy in rare cases of unexplained alopecia.
Based on findings, treatment plans may combine:
- Medical therapies – topical steroids, oral antifungals, hormone modulators.
- Procedural options – platelet‑rich plasma (PRP) injections, mesotherapy, or hair transplant surgery for permanent restoration.
- Supportive care – gentle shampoos, scalp massage, stress‑management techniques.
Gold City Medical Center offers an integrative approach, blending evidence‑based medicine with aesthetic expertise to address both the physical and emotional impact of scalp pain and hair loss.
Lifestyle Factors and Home Care Strategies
Everyday habits can either soothe or aggravate scalp discomfort. Simple adjustments often provide noticeable relief and support hair regrowth.
- Gentle cleansing – Use sulfate‑free shampoos with anti‑inflammatory ingredients such as aloe vera or tea tree oil.
- Scalp massage – 5‑minute daily massage with fingertips or a soft brush improves circulation and reduces tension.
- Balanced nutrition – Adequate protein, iron, zinc, and omega‑3 fatty acids are essential for robust follicle function.
- Stress reduction – Practices like mindfulness, yoga, or regular exercise lower cortisol levels that can trigger telogen shedding.
- Avoid harsh styling – Limit heat tools, tight ponytails, and chemical treatments that can inflame the scalp.
For those experiencing persistent itching or burning, applying a cool compress or using a fragrance‑free, hypoallergenic scalp serum can provide immediate comfort while the underlying cause is addressed.
Why Choose Gold City Medical Center
Gold City Medical Center combines advanced medical expertise with a holistic approach to hair restoration. Our team of dermatologists, trichologists, and cosmetic specialists works together to diagnose the root cause of scalp pain and hair loss and design personalized treatment plans. With state‑of‑the‑art facilities, minimally invasive procedures, and a commitment to patient comfort, we help you regain confidence and scalp health.
Ready to relieve scalp discomfort and restore your hair? Contact Gold City Medical Center today to schedule a comprehensive evaluation and take the first step toward a healthier scalp.
FAQ
What are the most common causes of scalp pain and hair loss?
Common causes include inflammatory skin disorders, traction alopecia, infections, medication side effects, and physical trauma.
How do dermatological conditions like alopecia areata affect hair growth?
Alopecia areata is an autoimmune attack on hair follicles, causing sudden patchy loss and sometimes scalp soreness.
What role do hormones and genetics play in hair loss?
Genetic sensitivity to DHT and hormonal changes like estrogen decline or thyroid imbalance drive pattern hair loss and can cause scalp discomfort.
When should someone seek professional evaluation for scalp pain?
If pain lasts more than two weeks, is accompanied by swelling, pus, or rapid hair loss, a specialist should be consulted.
What home‑care strategies can help relieve scalp discomfort?
Gentle cleansing, scalp massage, balanced nutrition, stress reduction, and avoiding harsh styling can improve scalp health.
What treatment options does Gold City Medical Center offer for scalp pain and hair loss?
The center provides medical therapies, procedural options like PRP, and supportive care tailored to each patient.