When you ask what is psoriasis, you are looking for a clear explanation of a common yet often misunderstood skin condition. Psoriasis is a chronic, immune‑mediated disease that speeds up the growth cycle of skin cells, leading to thick, red, scaly patches that can appear anywhere on the body. Around 2–3% of the global population lives with psoriasis, making it one of the most prevalent inflammatory skin disorders.
This article breaks down the essential aspects of psoriasis: its underlying causes, the main clinical types, typical symptoms, and the range of treatment options available today. Whether you are newly diagnosed, managing flare‑ups, or simply curious, understanding the condition helps you make informed decisions about care.
We will also explore lifestyle adjustments that can lessen the impact of psoriasis and highlight why Gold City Medical Center is equipped to provide comprehensive, integrative care for this condition.
Understanding Psoriasis: Definition and Causes
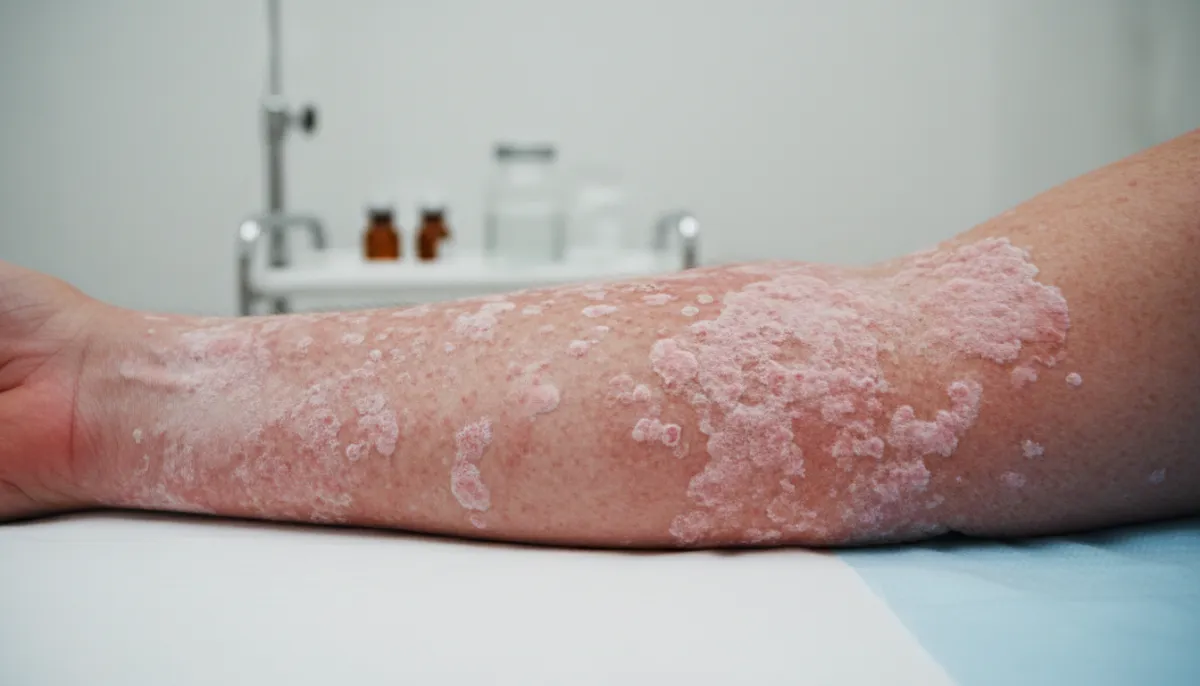
Psoriasis is fundamentally an autoimmune disease in which the immune system mistakenly attacks healthy skin cells. This triggers an overproduction of skin cells, causing them to accumulate on the surface faster than they can shed. The exact cause is multifactorial, involving genetic predisposition, environmental triggers, and immune dysregulation.
Autoimmune Basis
The immune system’s T‑cells become overactive, releasing cytokines such as TNF‑α, IL‑17, and IL‑23. These inflammatory signals accelerate keratinocyte proliferation, resulting in the hallmark plaques.
Genetic and Environmental Triggers
Research shows that up to 40% of people with psoriasis have a first‑degree relative with the condition, indicating a strong hereditary component. Environmental factors that can provoke or worsen the disease include:
- Stress and emotional trauma
- Skin injuries (the Koebner phenomenon)
- Infections, especially streptococcal throat infections
- Smoking and excessive alcohol consumption
- Obesity and metabolic syndrome
The table below summarizes the most common triggers and their typical impact on disease activity:
| Trigger | Effect on Psoriasis |
|---|---|
| Genetic predisposition | Increases baseline risk; may determine severity |
| Stress | Can precipitate flare‑ups within days |
| Infection (streptococcal) | Often initiates guttate psoriasis in children |
| Smoking | Associated with higher prevalence of plaque psoriasis |
| Obesity | Elevates systemic inflammation, worsening lesions |
Understanding these factors helps patients and clinicians target both medical and lifestyle interventions to keep the disease under control.
Common Types of Psoriasis and Their Characteristics
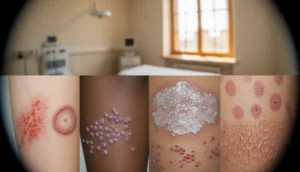
Psoriasis manifests in several distinct patterns, each with unique clinical features. Recognizing the type you have is essential for selecting the most effective treatment.
Plaque Psoriasis
Plaque psoriasis is the most common form, accounting for about 80% of cases. It presents as well‑defined, raised, red plaques covered with silvery‑white scales, often on the elbows, knees, scalp, and lower back.
Scalp Psoriasis
When lesions appear primarily on the scalp, they may be mistaken for dandruff. Scalp psoriasis can cause itching, flaking, and even hair loss if severe.
Guttate Psoriasis
Typically triggered by a streptococcal infection, guttate psoriasis produces small, drop‑shaped lesions on the trunk and limbs, frequently affecting children and young adults.
Inverse Psoriasis
Also known as flexural psoriasis, this type affects skin folds such as under the breasts, groin, or armpits. Lesions are smooth, red, and often aggravated by friction and sweating.
Pustular and Erythrodermic Psoriasis
These are less common but more severe forms. Pustular psoriasis features white pustules surrounded by red skin, while erythrodermic psoriasis involves widespread redness and shedding, potentially requiring hospitalization.
Below is a quick comparison of the major types:
| Type | Typical Appearance | Common Locations | Triggers |
|---|---|---|---|
| Plaque | Raised red plaques with silvery scales | Elbows, knees, scalp, lower back | Genetics, stress, injury |
| Scalp | Red, flaky patches on scalp | Scalp only | Weather changes, hair products |
| Guttate | Small drop‑shaped lesions | Trunk, limbs | Streptococcal infection |
| Inverse | Smooth red patches | Skin folds | Friction, heat |
| Pustular | White pustules on red base | Hands, feet, generalized | Medications, infections |
Recognizing Psoriasis Symptoms and When to Seek Help
Early identification of psoriasis symptoms can prevent misdiagnosis and allow prompt treatment. While the condition primarily affects the skin, it can also involve nails, scalp, and joints.
Skin Manifestations
Key skin signs include:
- Red, inflamed patches that may itch or burn
- Silvery‑white scaling that is often more noticeable after a shower
- Sharp borders separating affected skin from healthy tissue
Nail Involvement
Up to 50% of patients develop nail changes such as pitting, thickening, or separation of the nail from the nail bed (onycholysis). These signs are especially common in psoriasis on the nails.
Scalp and Facial Areas
Scalp involvement can cause persistent dandruff‑like flaking, while facial lesions may appear as small, red plaques around the eyebrows, beard area, or behind the ears.
Joint Symptoms (Psoriatic Arthritis)
Approximately 30% of individuals with psoriasis experience joint pain, stiffness, and swelling—a condition known as psoriatic arthritis. Early detection is crucial to prevent joint damage.
If you notice any of these signs, especially a sudden flare after a throat infection or a new area of scaling, it is advisable to consult a dermatologist. Timely professional evaluation can differentiate psoriasis from eczema, fungal infections, or other skin disorders.
Treatment Options: From Topical Creams to Advanced Therapies
Managing psoriasis involves a stepwise approach that starts with the least invasive options and progresses to systemic or biologic therapies when needed. Treatment goals are to reduce inflammation, clear skin lesions, and improve quality of life.
Topical Therapies
First‑line treatments often include:
- Corticosteroid creams – reduce inflammation quickly but should be used short‑term.
- Vitamin D analogues (e.g., calcipotriene) – slow skin cell growth.
- Combination products (steroid + vitamin D) – offer synergistic benefits.
- Coal tar and salicylic acid – useful for scalp psoriasis.
Phototherapy
Controlled exposure to ultraviolet B (UVB) light can improve moderate plaque psoriasis. Narrowband UVB is the most commonly used modality, typically administered 2–3 times per week.
Systemic Medications
For extensive disease, oral or injectable systemic drugs are prescribed, such as:
- Methotrexate – a folate antagonist that dampens immune activity.
- Cyclosporine – a potent immunosuppressant for short‑term control.
- Acitretin – a retinoid that normalizes skin cell growth.
Biologic Therapies
Biologics target specific immune pathways (TNF‑α, IL‑17, IL‑23) and have transformed the management of severe psoriasis and psoriatic arthritis. Examples include adalimumab, secukinumab, and ustekinumab. These agents are administered via injection and require monitoring for infections.
The comparison table outlines when each treatment category is typically considered:
| Therapy | Indication | Typical Use | Key Considerations |
|---|---|---|---|
| Topical creams | Mild to moderate plaques | Daily application | Skin irritation possible |
| Phototherapy | Moderate disease, especially on trunk | 2–3 sessions/week | Requires clinic visits |
| Systemic meds | Extensive or refractory psoriasis | Oral or injectable | Monitor liver, kidney, blood counts |
| Biologics | Severe plaque psoriasis or psoriatic arthritis | Injectable every 2–4 weeks | Screen for TB, hepatitis |
Choosing the right regimen depends on disease severity, location, patient preference, and any co‑existing health conditions. A dermatologist can tailor a plan that balances efficacy with safety.
Living with Psoriasis: Lifestyle Tips and Support
Medical treatment is only part of a comprehensive psoriasis management plan. Lifestyle choices can markedly influence flare‑ups and overall wellbeing.
Diet and Nutrition
While no single diet cures psoriasis, certain foods may help reduce inflammation:
- Omega‑3 rich fish (salmon, mackerel)
- Colorful fruits and vegetables high in antioxidants
- Whole grains and legumes
- Limiting processed foods, red meat, and sugary drinks
Stress Management
Stress is a well‑documented trigger. Techniques such as mindfulness meditation, yoga, deep‑breathing exercises, and regular physical activity can lower cortisol levels and improve skin outcomes.
Skin Care Routine
Gentle skin care helps maintain barrier function:
- Use lukewarm water and fragrance‑free moisturizers immediately after bathing.
- Avoid harsh soaps, scrubs, and prolonged hot showers.
- Consider medicated shampoos for scalp involvement.
Support Networks
Connecting with others living with psoriasis can provide emotional relief and practical advice. Online forums, patient advocacy groups, and local support meetings are valuable resources.
By integrating medical therapy with healthy habits and community support, many individuals achieve long‑term control of their symptoms and a better quality of life.
Why Choose Gold City Medical Center for Psoriasis Care
Gold City Medical Center combines cutting‑edge dermatological expertise with an integrative approach that addresses both medical and lifestyle aspects of psoriasis. Our team of board‑certified specialists offers personalized treatment plans, ranging from topical regimens to advanced biologic therapies, all within a compassionate, patient‑focused environment. With state‑of‑the‑art facilities and a commitment to continuous education, we empower you to manage psoriasis effectively and confidently.
Ready to take control of your skin health? Contact Gold City Medical Center today to schedule a comprehensive dermatology consultation and discover a treatment plan tailored to your needs.
Call us or visit our clinic for a personalized assessment and start your journey toward clearer, healthier skin.
FAQ
What causes psoriasis?
Psoriasis is caused by a combination of genetic predisposition, immune system dysfunction, and environmental triggers such as stress, infection, and lifestyle factors.
What are the different types of psoriasis?
The main types are plaque, scalp, guttate, inverse, pustular, and erythrodermic psoriasis, each with distinct appearance and typical locations.
How can I tell if I have psoriasis or another skin condition?
Key signs of psoriasis include well‑defined red patches with silvery scaling, sharp borders, and possible nail or joint involvement, which differ from eczema or fungal infections.
What treatment options are available for psoriasis?
Treatments range from topical creams and phototherapy to systemic medications and biologic therapies, chosen based on severity and patient needs.
When should I see a dermatologist for psoriasis?
Consult a dermatologist if you notice new or worsening patches, experience joint pain, or if over‑the‑counter treatments fail to improve your skin.
Can lifestyle changes help manage psoriasis?
Yes, stress reduction, a healthy diet, weight management, and avoiding smoking and excess alcohol can lessen flare‑ups and improve treatment response.