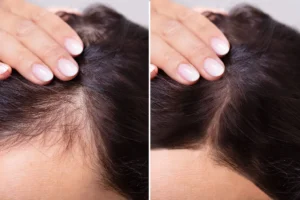
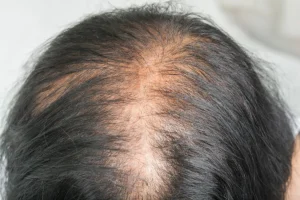
Many patients wonder, does immunotherapy cause hair loss, especially when they are starting a new cancer treatment plan. Understanding the relationship between modern immune‑based therapies and hair health is essential for making informed decisions and preparing for potential side effects.
Immunotherapy has transformed oncology by harnessing the body’s own immune system to target cancer cells. While it is celebrated for its precision, it also brings a unique profile of side effects that differ from traditional chemotherapy. Hair loss is one of the concerns that frequently surfaces during patient consultations.
Recent studies suggest that up to 20% of patients receiving certain checkpoint inhibitors report some degree of hair thinning or shedding. This figure is lower than the 80‑90% hair loss rate commonly associated with conventional chemotherapy, but the impact on quality of life can still be significant.
In this article, we will explore how immunotherapy works, why hair loss may occur, how it compares to other cancer treatments, and practical strategies to protect and regrow your hair. Whether you are considering immunotherapy, currently undergoing treatment, or supporting a loved one, the information below will help you navigate this complex topic with confidence.
How Immunotherapy Works and Why Hair Loss May Occur
Immunotherapy activates the immune system to recognize and destroy cancer cells. The most common classes include checkpoint inhibitors, CAR‑T cell therapy, and cytokine treatments. By blocking proteins such as PD‑1, PD‑L1, or CTLA‑4, these drugs release the “brakes” on T‑cells, allowing them to attack tumors more effectively.
Although the primary target is cancer, the heightened immune activity can inadvertently affect normal tissues, including hair follicles. The mechanisms behind hair loss in immunotherapy patients are still being studied, but two main pathways have been identified:
- Autoimmune‑like reactions: The immune system may mistakenly target hair follicle cells, leading to inflammation and temporary shedding.
- Cytokine‑induced stress: Elevated levels of inflammatory cytokines (e.g., interferon‑γ, interleukin‑6) can disrupt the hair growth cycle, pushing follicles into the telogen (resting) phase.
These processes differ from the direct cytotoxic damage caused by chemotherapy, which attacks rapidly dividing cells—including those in the hair matrix—resulting in more extensive hair loss.
It is important to note that not all immunotherapy agents carry the same risk. For example, pembrolizumab and nivolumab have reported lower rates of alopecia compared with ipilimumab, which is more frequently associated with autoimmune skin reactions.

Comparing Immunotherapy Side Effects to Chemotherapy
When evaluating treatment options, patients often compare immunotherapy side effects with those of chemotherapy. While both aim to eradicate cancer, their toxicity profiles are distinct.
Below is a concise comparison of the most common adverse events associated with each modality:
| Side Effect | Immunotherapy | Chemotherapy |
|---|---|---|
| Haaruitval | Usually mild or patchy; does immunotherapy cause hair loss in a minority of patients | Often severe and diffuse; up to 90% of patients |
| Vermoeidheid | Common, often manageable | Frequent and can be profound |
| Skin Reactions | Rash, vitiligo‑like depigmentation | Hand‑foot syndrome, alopecia |
| Gastrointestinal Issues | Colitis, diarrhea (immune‑mediated) | Nausea, vomiting, mucositis |
| Endocrine Disorders | Hypothyroidism, adrenal insufficiency | Less common |
Understanding these differences helps patients anticipate which side effects they might need to manage. While chemotherapy’s hair loss is predictable and often total, immunotherapy‑related hair shedding tends to be unpredictable, sometimes appearing as localized patches or diffuse thinning.
Patients who are particularly concerned about hair preservation may opt for immunotherapy when clinically appropriate, but they should still discuss potential risks with their oncologist.
Managing Hair Loss During Immunotherapy Treatment
Even though the risk is lower, hair loss during immunotherapy can still be distressing. Proactive measures can reduce shedding and support overall scalp health.
Medische ingrepen
- Topical steroids: Reduce inflammation around hair follicles when autoimmune reactions are identified.
- Minoxidil (Rogaine): May stimulate hair regrowth in the telogen phase; consult your dermatologist before use.
- Low‑dose oral corticosteroids: Prescribed for severe immune‑mediated alopecia, but balanced against potential systemic effects.
Lifestyle and Cosmetic Strategies
- Gentle hair care: Use sulfate‑free shampoos, avoid tight hairstyles, and limit heat styling.
- Scalp massage: Improves blood flow and may encourage follicle activity.
- Wigs and hairpieces: Modern, breathable options can boost confidence during treatment.
- Nutrition: Adequate protein, iron, zinc, and biotin support healthy hair growth.
It is also essential to differentiate between hair loss caused by immunotherapy and that resulting from other concurrent treatments, such as radiation therapy or hormone therapy. For instance, does radiation cause hair loss is a common question; radiation can lead to localized hair loss in the treated field, which may overlap with immunotherapy‑related shedding.
Regular communication with your oncology team enables early detection of hair‑related side effects and timely adjustment of supportive care.
What to Expect After Treatment: Hair Regrowth and Recovery
After completing immunotherapy, most patients experience gradual hair regrowth. The timeline varies, but typical patterns include:
- Initial shedding may cease within weeks of treatment completion.
- Fine, often lighter‑colored hair may begin to grow within 2‑3 months.
- Full density and normal texture often return within 6‑12 months, though some individuals notice lasting changes.
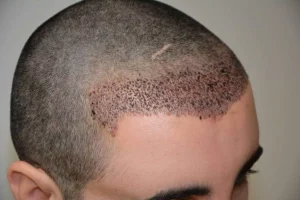
Factors influencing regrowth speed include age, overall health, nutritional status, and whether additional therapies (e.g., chemotherapy or radiation) were administered. In cases where hair does not fully recover, options such as hair transplantation—one of the specialties at Gold City Medical Center—can provide permanent restoration.
Patients should continue scalp‑friendly practices and consider periodic dermatology visits to monitor progress. If hair growth is slow, low‑level laser therapy or platelet‑rich plasma (PRP) injections are emerging adjuncts that may accelerate follicular activity.
Additional Factors Influencing Hair Health in Cancer Care
Hair health is not solely determined by the type of cancer therapy. Several other variables can contribute to shedding or thinning:
Radiation Therapy
Localized radiation can damage hair follicles in the treatment field, leading to permanent alopecia in some cases. The severity depends on dose, fractionation, and individual sensitivity. While does radiation therapy make you lose your hair is a frequent concern, modern techniques such as intensity‑modulated radiation therapy (IMRT) aim to spare surrounding healthy tissue.
Hormone Treatments
Certain endocrine therapies, especially those used in breast and prostate cancer, can cause hormonal imbalances that affect hair cycles. Patients may notice thinning similar to androgenic alopecia.
Stress and Nutrition
Psychological stress, common during a cancer diagnosis, can trigger telogen effluvium—a temporary shedding of hair. Maintaining a balanced diet rich in vitamins (A, C, D, E) and minerals supports follicle resilience.
Finally, some patients report hair loss as a symptom of the underlying disease itself, not just the treatment. Continuous monitoring and a multidisciplinary approach ensure that all potential causes are addressed.
Why Choose Gold City Medical Center
Gold City Medical Center combines cutting‑edge oncology expertise with a holistic approach to patient wellbeing. Our team of experienced oncologists, dermatologists, and hair restoration specialists work together to create personalized treatment plans that address both cancer control and quality‑of‑life concerns such as hair health. With state‑of‑the‑art facilities and a commitment to evidence‑based care, we provide comprehensive support—from managing immunotherapy side effects to offering advanced hair transplantation for lasting results.
Ready to discuss how immunotherapy may affect your hair and explore protective strategies? Contact Gold City Medical Center today to schedule a personalized consultation. Take the next step toward confident, comprehensive care.
FAQ
Does immunotherapy cause hair loss?
Yes, a minority of patients (about 20%) experience hair thinning or shedding during immunotherapy.
How does hair loss from immunotherapy differ from chemotherapy?
Immunotherapy‑related hair loss is typically milder, patchy, and caused by immune reactions, while chemotherapy causes severe, diffuse loss by killing rapidly dividing hair‑matrix cells.
What are the common side effects of immunotherapy?
Typical immunotherapy side effects include fatigue, skin rashes, colitis, endocrine disorders, and occasionally mild hair loss.
How can I manage hair loss during immunotherapy?
Use gentle hair care, topical steroids, minoxidil, low‑dose oral corticosteroids, and consider wigs or scalp‑friendly nutrition.
When can I expect my hair to grow back after immunotherapy?
Hair regrowth usually begins 2‑3 months after treatment ends and may reach full density within 6‑12 months.
Can radiation therapy also cause hair loss?
Yes, radiation can cause localized hair loss in the treated area, sometimes permanently.
What treatments are available for immunotherapy‑induced alopecia?
Topical steroids, minoxidil, low‑dose oral corticosteroids, and in refractory cases, hair transplantation are options.
Are there preventive measures to protect hair during immunotherapy?
Gentle hair care, scalp massage, balanced nutrition, and early communication with the oncology team can help preserve hair.