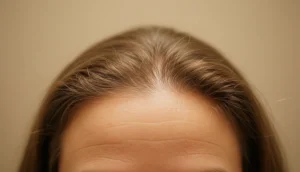
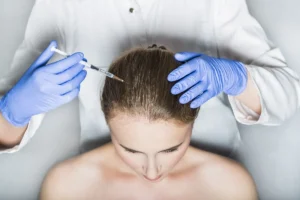
Understanding telogen effluvium before and after is essential for anyone experiencing sudden hair shedding, especially when stress or hormonal changes are involved. This article explains what telogen effluvium is, how to recognize the early signs, the treatment pathways available, and what you can expect once the shedding phase ends. By demystifying the condition, we aim to empower patients to seek timely help and regain confidence in their hair health.
Hair loss affects millions worldwide, but not all shedding is permanent. In fact, telogen effluvium accounts for up to 30% of diffuse hair loss cases seen in dermatology clinics. The condition is typically triggered by physiological stressors such as illness, surgery, severe emotional stress, or drastic hormonal shifts. While the experience can be unsettling, most individuals see hair regrowth within months once the underlying cause is addressed.
In the sections that follow, we will walk through the typical timeline of telogen effluvium, discuss practical strategies to minimise shedding, and outline evidence‑based treatments that can accelerate recovery. Whether you are curious about the “before” phase, the “after” results, or both, the information here is designed to be clear, actionable, and aligned with the integrative care approach of Gold City Medical Center.
What Is Telogen Effluvium?

Telogen effluvium is a form of non‑scarring hair loss that occurs when a large number of hair follicles prematurely enter the telogen (resting) phase. Under normal conditions, only about 5–10% of scalp hairs are in telogen at any given time. When a trigger such as severe stress, a fever, or a rapid weight loss event occurs, this proportion can rise sharply, leading to noticeable shedding.
The condition is distinct from androgenetic alopecia, which is a permanent thinning pattern driven by genetics and hormones. Because telogen effluvium does not damage the follicle permanently, hair typically regrows once the disruptive factor is removed. However, the shedding can be alarming, especially when it appears suddenly across the crown or along the hairline.
Key factors that can precipitate telogen effluvium include:
- Physical stress: major surgery, high fever, or chronic illness.
- Emotional stress: bereavement, job loss, or intense anxiety.
- Hormonal changes: postpartum period, thyroid disorders, or contraceptive adjustments.
- Nutritional deficiencies: iron, zinc, or protein shortage.
- Medications: anticoagulants, retinoids, or certain antidepressants.
Understanding these triggers helps clinicians tailor a personalized treatment plan that addresses both the cause and the symptoms.
Recognizing the Signs: Before the Shedding Starts
Before the visible shedding begins, many patients notice subtle cues that hint at an upcoming telogen phase. These early indicators are crucial for early intervention.
Hair shedding often starts 2–3 months after the inciting event. During this latency period, the hair follicles are already transitioning, but the hair shaft has not yet been expelled. Common pre‑shedding symptoms include:
- Increased hair on pillows or in the shower drain.
- Feeling of overall hair thinning, especially at the crown.
- Mild scalp itching or tingling sensations.
- Noticeable increase in hairs when combing or brushing.
To help patients differentiate telogen effluvium from other forms of hair loss, clinicians often use a simple “pull test.” By gently tugging a small cluster of hairs, they can assess how many hairs come out; a positive result (more than 10% of pulled hairs) supports the diagnosis.
| Indicator | Typical Timing | Clinical Relevance |
|---|---|---|
| Stressful event (surgery, illness) | 0–2 weeks | Trigger for follicular shift |
| Latency period (no visible shedding) | 2–3 months | Opportunity for early counseling |
| Visible shedding begins | 3–4 months | Confirm diagnosis, start treatment |
Recognising these signs early can reduce the duration of the shedding phase and improve overall outcomes.
Managing the Shedding: Treatment Options and Lifestyle Changes
Once telogen effluvium is diagnosed, the primary goal is to halt further shedding and create an environment that supports regrowth. Treatment is typically multifaceted, combining medical, nutritional, and lifestyle interventions.
Medical interventions may include:
- Topical minoxidil (2% or 5%) to stimulate follicular activity.
- Low‑dose oral corticosteroids for severe inflammatory triggers.
- Iron supplementation if laboratory tests reveal deficiency.
- Thyroid hormone replacement when hypothyroidism is identified.
In addition to medication, lifestyle adjustments play a pivotal role. Reducing chronic stress through mindfulness, yoga, or counseling can curb the hormonal cascade that fuels hair shedding. Adequate protein intake (1.2–1.5 g per kilogram of body weight) and a balanced diet rich in vitamins A, C, D, E, zinc, and biotin provide the building blocks for healthy hair shafts.
Scalp care is another cornerstone. Gentle shampoos, avoiding heat styling, and periodic scalp massages improve blood flow, delivering nutrients more efficiently to the follicles.
Below is a quick reference of common treatment modalities and their typical duration of use:
| Treatment | Typical Duration | Key Benefit |
|---|---|---|
| Topical Minoxidil | 6–12 months | Stimulates follicle proliferation |
| Iron Supplementation | 3–6 months | Corrects deficiency‑related shedding |
| Stress‑Management Programs | Ongoing | Reduces cortisol‑driven hair loss |
| Protein‑Rich Diet | Continuous | Provides essential amino acids for hair growth |
Patients who adhere to a comprehensive plan often notice a reduction in shedding within 8–12 weeks, although full recovery may take longer.
What to Expect After Recovery: The After Phase
After the shedding period subsides, the scalp enters the anagen (growth) phase, and new hairs begin to appear. The “after” stage can be divided into three observable milestones:
- Initial regrowth (1–3 months): Fine, often lighter hairs emerge, creating a subtle improvement in density.
- Mid‑term thickening (4–6 months):> The new hairs gain pigment and thickness, making the scalp appear fuller.
- Full restoration (6–12 months):> Hair density approaches pre‑shedding levels, and the overall texture normalises.
It is normal for the early regrowth hairs to be thinner and more fragile. Patience and continued scalp care are essential during this phase. In some cases, patients may experience a “mini‑rebound” where a small amount of shedding recurs as the follicle cycle stabilises; this typically resolves without further intervention.
Monitoring progress with photographic documentation can be motivating and also helps clinicians adjust treatment if regrowth stalls. If after a year there is still significant thinning, additional options such as platelet‑rich plasma (PRP) therapy or hair transplant consultation may be explored.
Supporting Hair Regrowth: Nutrition, Scalp Care, and Professional Help
Beyond medical treatment, long‑term hair health relies on a holistic approach that integrates nutrition, scalp hygiene, and regular professional assessments.
Nutrition should focus on:
- Lean proteins (fish, poultry, legumes) for keratin synthesis.
- Omega‑3 fatty acids (salmon, flaxseed) to reduce inflammation.
- Vitamin‑rich foods: leafy greens for iron, citrus fruits for vitamin C, nuts for zinc.
- Adequate hydration to maintain cellular function.
Scalp care routines that complement treatment include:
- Using a mild, sulfate‑free shampoo to avoid irritation.
- Applying a lightweight, peptide‑based serum that promotes circulation.
- Massaging the scalp for 5 minutes daily to enhance blood flow.
- Limiting heat styling and harsh chemical treatments.
Professional services offered at Gold City Medical Center, such as low‑level laser therapy and PRP injections, can accelerate the regenerative process, especially for patients with prolonged shedding or slower regrowth.
By combining evidence‑based medical options with lifestyle optimisation, most individuals experience a complete reversal of telogen effluvium, returning to a fuller, healthier head of hair.
Why Choose Gold City Medical Center
Gold City Medical Center delivers integrative care that blends cutting‑edge medical treatments with personalized wellness strategies. Our multidisciplinary team includes dermatologists, trichologists, and nutrition specialists who work together to identify the root cause of hair loss and design a tailored recovery plan. With a focus on patient education, state‑of‑the‑art facilities, and compassionate support, we help clients navigate telogen effluvium from the “before” phase through lasting “after” results.
Ready to restore your hair confidence? Contact Gold City Medical Center today for a comprehensive evaluation and a customised treatment roadmap. Take the first step toward healthier hair and a brighter tomorrow.
FAQ
What causes telogen effluvium?
Telogen effluvium is triggered by physical or emotional stress, hormonal changes, nutritional deficiencies, and certain medications.
How can I recognize the early signs of telogen effluvium before shedding starts?
Early signs include increased hair on pillows or in the shower, a feeling of thinning, mild scalp itching, and more hairs coming out during brushing.
What treatment options are available for telogen effluvium?
Treatment combines medical interventions like minoxidil, corticosteroids, iron or thyroid supplements, with lifestyle changes such as stress management and nutrition.
How long does it take for hair to regrow after telogen effluvium?
Initial regrowth appears in 1–3 months, with noticeable thickening by 4–6 months, and near‑full restoration by 6–12 months.
Can nutrition and lifestyle changes help with telogen effluvium recovery?
Yes, a balanced diet rich in protein, iron, zinc, and omega‑3s, along with stress‑reduction practices, supports faster hair regrowth.
When should I consider professional therapies like PRP or laser treatment?
If significant thinning persists after 12 months of conservative treatment, consulting for PRP or low‑level laser therapy is advisable.