When you notice more strands on your pillow each morning, you may wonder which tests for hair thinning can pinpoint the cause. At Gold City Medical Center, we combine medical expertise with cutting‑edge technology to diagnose hair loss accurately. Early detection is essential because it opens the door to targeted treatments that can halt or even reverse thinning. In fact, studies show that up to 70 % of hair loss cases are treatable when identified promptly.
This article walks you through the most common diagnostic tools, from simple blood panels to advanced scalp imaging. You’ll learn what each test measures, why it matters, and how the results guide personalized treatment plans. Whether you’re dealing with telogen effluvium, androgen‑dependent alopecia, or another form of thinning, understanding the diagnostic process empowers you to make informed decisions about your hair health.
We’ll also explore how the results of these examinations translate into actionable steps, including medical therapies, lifestyle adjustments, and surgical options like hair transplantation. By the end, you’ll have a clear roadmap for navigating the journey from concern to confidence.
Common Methods to Diagnose Hair Thinning
Before ordering specialized laboratory work, clinicians often start with a thorough clinical evaluation. This initial assessment helps narrow down potential causes and determines which hair thinning tests are most appropriate.
- Medical History Review: A detailed questionnaire covering family history, diet, stress levels, medications, and previous hair‑related conditions.
- Physical Scalp Examination: Visual inspection and palpation to assess hair density, scalp health, and patterns of loss.
- Pull Test: Gentle tug on a small bundle of hair to gauge shedding rate; a positive result often indicates active hair loss.
- Phototrichogram: High‑resolution photographs taken at baseline and after a set interval to track hair growth cycles.
These foundational steps are crucial because they help clinicians decide whether further laboratory or imaging studies are needed. For many patients, the combination of history and physical exam already provides valuable clues about whether the thinning is due to hormonal changes, nutritional deficiencies, or an underlying medical condition.
Laboratory Tests: What They Reveal
Laboratory analysis is a cornerstone of the diagnostic pathway for hair thinning. Blood work can uncover systemic issues that may be silently contributing to follicle miniaturization. Below is a concise table summarizing the most frequently ordered tests and the insights they provide.
| Test | What It Measures | Relevance to Hair Thinning |
|---|---|---|
| Complete Blood Count (CBC) | Red and white blood cell levels, hemoglobin | Detects anemia, which can cause diffuse hair shedding. |
| Ferritin | Iron storage protein | Low ferritin is linked to telogen effluvium and reduced hair growth. |
| Thyroid Panel (TSH, Free T4) | Thyroid hormone activity | Both hyper- and hypothyroidism can trigger hair thinning. |
| Sex Hormones (Testosterone, DHT, Estradiol) | Androgen and estrogen levels | Elevated DHT is a primary driver of androgenetic alopecia. |
| Vitamine D | Serum 25‑OH vitamin D | Deficiency may impair follicular cycling and lead to thinning. |
| Zinc & Selenium | Essential trace minerals | Deficiencies can cause fragile hair shafts and increased shedding. |
These laboratory hair thinning examinations are typically ordered together as a panel to provide a comprehensive picture. The results help clinicians differentiate between nutritional deficiencies, hormonal imbalances, and autoimmune disorders, each of which may require a distinct therapeutic approach.
Scalp Imaging and Trichoscopy
Visualizing the scalp at a microscopic level offers unparalleled insight into hair follicle health. Trichoscopy, also known as scalp dermoscopy, is a non‑invasive imaging technique that magnifies the scalp up to 70×, revealing patterns that are invisible to the naked eye.
- Hair Shaft Diameter Variation: Detects miniaturized hairs typical of androgenetic alopecia.
- Perifollicular Inflammation: Indicates an autoimmune component such as alopecia areata.
- Yellow Dots and Black Puncta: Markers of sebaceous gland activity and fungal infection, respectively.
- Vascular Patterns: Abnormal blood vessel networks may suggest chronic scalp conditions.
High‑resolution trichoscopic images are captured and stored for longitudinal comparison, allowing clinicians to monitor treatment response over weeks or months. In addition to trichoscopy, other imaging modalities like the phototrichogram and 3‑D scalp scanning provide quantitative data on hair density and growth rates.
Genetic and Hormonal Assessments
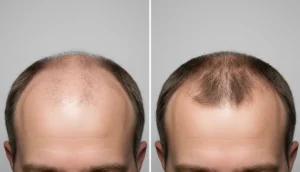
Genetic predisposition plays a significant role in many forms of hair loss, especially male and female pattern baldness. DNA testing can identify specific gene variants linked to increased DHT sensitivity, helping predict the likelihood of progressive thinning.
- Androgen Receptor Gene (AR) Polymorphisms: Variants that amplify DHT’s effect on follicles.
- Wnt Signaling Pathway Markers: Influence hair follicle regeneration and cycling.
- Hormone Level Panels: In addition to the basic thyroid and sex hormone tests, specialized assays for cortisol and prolactin can uncover stress‑related or pituitary causes.
When genetic testing reveals a high risk of androgen‑driven alopecia, clinicians may recommend early intervention with medications such as finasteride or topical minoxidil, alongside lifestyle modifications. Hormonal assessments, especially for women, also guide the use of anti‑androgen therapies or estrogen supplementation when appropriate.
Interpreting Results and Planning Treatment
After completing the suite of hair thinning tests, the next critical step is translating data into a clear treatment roadmap. The interpretation process involves correlating clinical findings with laboratory and imaging results to pinpoint the primary drivers of hair loss.
- Identify Primary Etiology: Determine whether the thinning is primarily hormonal, nutritional, inflammatory, or a combination.
- Set Treatment Priorities: Address reversible factors first—e.g., iron supplementation for low ferritin or thyroid medication for hypothyroidism.
- Choose Targeted Therapies: Options include FDA‑approved medications (finasteride, minoxidil), platelet‑rich plasma (PRP) injections, or surgical hair transplantation.
- Monitor Progress: Schedule follow‑up trichoscopic imaging and repeat blood work every 3–6 months to assess efficacy.
- Adjust Plan as Needed: If initial therapies are ineffective, consider adjunctive treatments such as low‑level laser therapy or nutraceuticals.
Clear communication between patient and clinician is essential throughout this process. At Gold City Medical Center, we provide detailed reports and personalized counseling so you understand each step and feel confident in the chosen path.
Why Choose Gold City Medical Center
Gold City Medical Center combines integrative healthcare with state‑of‑the‑art diagnostics to deliver comprehensive solutions for hair thinning. Our multidisciplinary team includes dermatologists, endocrinologists, and hair restoration surgeons who collaborate to create individualized treatment plans. With a focus on evidence‑based medicine and patient‑centered care, we ensure that every test—whether a simple blood panel or an advanced trichoscopic scan—is interpreted within the broader context of your overall health. Trust our expertise to guide you from diagnosis to lasting results.
Ready to uncover the cause of your hair thinning? Contact Gold City Medical Center today to schedule a comprehensive assessment and take the first step toward healthier, fuller hair.
FAQ
What tests are used to diagnose hair thinning?
Diagnosis typically starts with a medical history review, physical scalp exam, pull test, and phototrichogram, followed by blood panels and scalp imaging.
How does a blood test help identify hair loss causes?
Blood tests detect anemia, iron deficiency, thyroid disorders, hormone imbalances, and nutrient deficiencies that can trigger hair shedding.
What is trichoscopy and why is it important for hair thinning diagnosis?
Trichoscopy is a non‑invasive scalp dermoscopy that magnifies the scalp up to 70×, revealing follicular patterns invisible to the naked eye.
Can genetic testing predict the risk of hair thinning?
Yes, DNA testing can identify gene variants, such as androgen receptor polymorphisms, that increase susceptibility to androgen‑driven hair loss.
What treatment options are available after the diagnostic tests?
Treatment may include FDA‑approved medications, PRP injections, lifestyle changes, low‑level laser therapy, nutraceuticals, or surgical hair transplantation.
Why choose Gold City Medical Center for hair thinning evaluation?
Gold City Medical Center offers an integrative team of dermatologists, endocrinologists, and surgeons with state‑of‑the‑art diagnostics and personalized care.